10 Airborne Diseases and the Conditions That Accelerate Their Spread
Airborne diseases represent one of humanity's most persistent and challenging health threats, traveling silently through the very air we breathe and crossing boundaries with unprecedented ease. These microscopic pathogens—including viruses, bacteria, fungi, and other microorganisms—exploit the fundamental necessity of respiration to infiltrate our bodies, making prevention particularly complex. Unlike vector-borne or contact-transmitted diseases, airborne pathogens can spread rapidly across vast distances, affecting entire communities within days or weeks. The transmission mechanisms vary from large respiratory droplets that settle quickly to microscopic aerosols that can remain suspended for hours, creating multiple pathways for infection. Environmental conditions, human behavior, architectural design, and population density all play crucial roles in either facilitating or hindering the spread of these diseases. Understanding the intricate relationship between airborne pathogens and the conditions that accelerate their transmission is essential for developing effective prevention strategies, designing safer public spaces, and preparing for future outbreaks. This comprehensive exploration examines ten significant airborne diseases alongside the environmental and social factors that create perfect storms for their proliferation, providing insights that are more relevant than ever in our interconnected world.
1. Tuberculosis - The Ancient Killer's Modern Resurgence

Tuberculosis remains one of the world's deadliest airborne diseases, with Mycobacterium tuberculosis causing approximately 1.5 million deaths annually despite being largely preventable and treatable. This ancient pathogen spreads through microscopic droplets expelled when infected individuals cough, sneeze, speak, or sing, with each infected person potentially transmitting the disease to 10-15 others in a year without proper treatment. The conditions that accelerate TB transmission are deeply intertwined with socioeconomic factors, creating a vicious cycle of poverty and disease. Overcrowded living conditions, particularly in urban slums, refugee camps, and correctional facilities, provide ideal environments for TB transmission, as the bacteria can survive in poorly ventilated spaces for extended periods. Malnutrition weakens immune systems, making individuals more susceptible to infection and progression from latent to active disease. HIV co-infection dramatically increases TB susceptibility, with HIV-positive individuals being 20-30 times more likely to develop active tuberculosis. Air pollution, both indoor from cooking fires and outdoor from industrial sources, damages respiratory systems and increases vulnerability. The emergence of drug-resistant strains, including multidrug-resistant (MDR-TB) and extensively drug-resistant (XDR-TB) variants, has complicated treatment efforts and increased transmission risks in healthcare settings where inadequate infection control measures exist.
2. Influenza - The Shape-Shifting Seasonal Threat

Influenza viruses demonstrate remarkable adaptability, continuously evolving through antigenic drift and shift to evade human immune responses, making them perpetual threats to global health. These RNA viruses spread primarily through respiratory droplets and aerosols, with infected individuals shedding virus particles for several days before and after symptom onset. Seasonal patterns of influenza transmission are closely linked to environmental conditions, with cold, dry air facilitating viral survival and transmission rates. Indoor crowding during winter months creates ideal conditions for spread, as people spend more time in enclosed spaces with reduced ventilation. Schools serve as major amplification sites, with children acting as efficient transmitters due to their close contact patterns and developing immune systems. International travel accelerates pandemic potential, as demonstrated by the 2009 H1N1 pandemic, which spread globally within months. Climate change is altering traditional seasonal patterns, potentially extending transmission seasons and shifting geographic distributions of different strains. Healthcare settings face particular challenges during influenza outbreaks, with hospital-acquired infections posing risks to vulnerable patients. The virus's ability to undergo reassortment in animal hosts, particularly pigs and birds, creates ongoing pandemic threats. Vaccination coverage rates significantly impact community transmission, with herd immunity thresholds varying by strain virulence and population demographics.
3. COVID-19 - Lessons from a Global Pandemic

The COVID-19 pandemic, caused by SARS-CoV-2, revolutionized our understanding of airborne disease transmission and highlighted the critical importance of environmental factors in pathogen spread. Initially thought to spread primarily through large droplets, research revealed that aerosol transmission plays a significant role, particularly in indoor environments with poor ventilation. The virus demonstrates remarkable stability in aerosols, remaining viable for hours in optimal conditions, which explains numerous superspreading events in restaurants, choirs, and fitness centers. Population density emerged as a critical factor, with urban areas experiencing rapid community transmission due to high contact rates and shared transportation systems. Age-related vulnerability patterns showed that while all ages could be infected, severe outcomes disproportionately affected older adults and those with underlying health conditions. Indoor air quality became paramount, with carbon dioxide levels serving as proxies for ventilation adequacy and infection risk. The role of asymptomatic and pre-symptomatic transmission complicated control efforts, as infected individuals unknowingly spread the virus during social interactions. Seasonal variations in transmission rates correlated with indoor activity levels and environmental conditions affecting viral stability. Healthcare worker infections highlighted the importance of proper personal protective equipment and ventilation systems in medical facilities. The pandemic demonstrated how quickly airborne diseases can overwhelm healthcare systems and disrupt global economies, emphasizing the need for robust preparedness strategies.
4. Measles - The Highly Contagious Childhood Threat
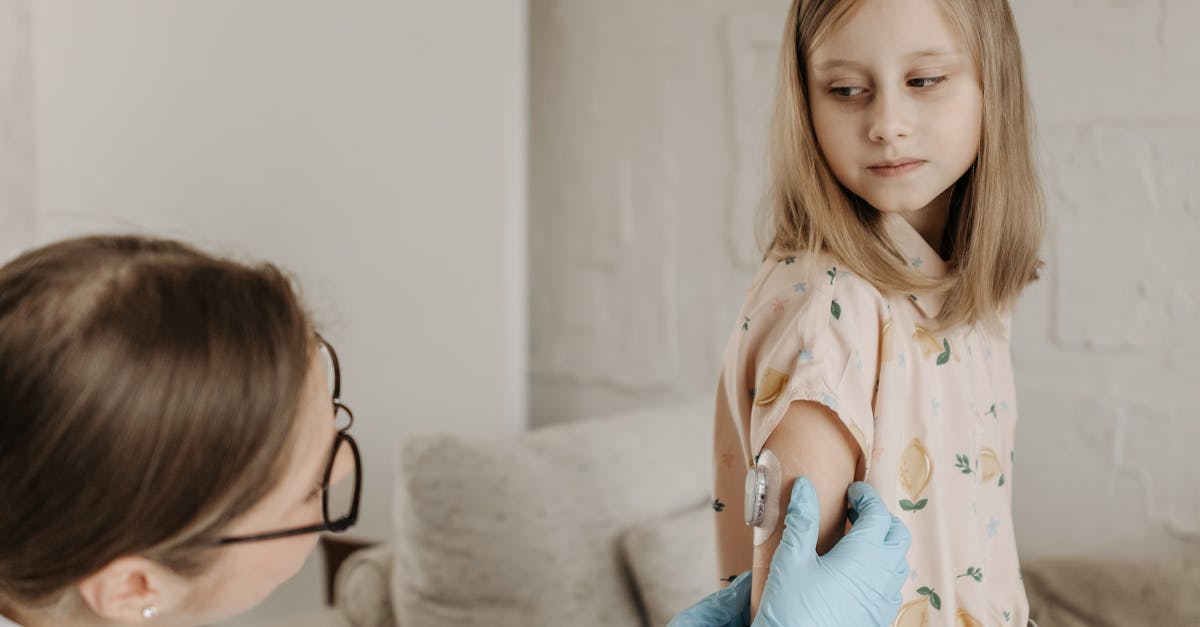
Measles, caused by the measles virus, ranks among the most contagious airborne diseases, with a basic reproduction number (R0) of 12-18, meaning each infected person can transmit the disease to 12-18 others in a completely susceptible population. The virus spreads through respiratory droplets and aerosols that can remain infectious in the air for up to two hours after an infected person leaves an area. Vaccination coverage rates directly impact transmission dynamics, with outbreaks occurring when immunization levels fall below the 95% threshold needed for herd immunity. School settings facilitate rapid transmission among unvaccinated children, with the virus spreading efficiently through classroom air circulation systems. International travel and migration patterns contribute to measles importation into countries with high vaccination coverage, often sparking outbreaks in communities with vaccine hesitancy. Poverty and healthcare access barriers create pockets of susceptible populations, particularly in developing countries where measles remains a leading cause of childhood mortality. Malnutrition, especially vitamin A deficiency, increases disease severity and mortality rates, creating cycles of vulnerability in affected communities. The virus's ability to cause temporary immunosuppression following infection increases susceptibility to secondary infections, compounding health impacts. Healthcare settings require strict airborne precautions due to the virus's high transmissibility and ability to infect healthcare workers. Climate factors, including seasonal patterns and population movement during certain times of year, influence outbreak timing and geographic spread patterns.
5. Legionnaires' Disease - The Environmental Opportunist

Legionnaires' disease, caused by Legionella pneumophila bacteria, represents a unique category of airborne illness that thrives in artificial water systems and spreads through contaminated aerosols. Unlike person-to-person transmitted diseases, Legionella requires specific environmental conditions to proliferate and become airborne, making it particularly associated with building systems and industrial processes. The bacteria multiply rapidly in warm water temperatures between 25-45°C (77-113°F), finding ideal habitats in cooling towers, hot water systems, decorative fountains, and spa pools. Biofilm formation within water systems provides protective environments where Legionella can survive disinfection attempts and continue multiplying. Aerosolization occurs when contaminated water is dispersed into fine droplets through showers, cooling towers, or misting systems, allowing bacteria to be inhaled deep into the lungs. Building design and maintenance practices significantly influence outbreak risks, with poorly maintained HVAC systems and water features serving as amplification sites. Age and immunocompromised status increase susceptibility, with elderly individuals and those with chronic lung diseases facing higher infection and mortality risks. Seasonal patterns often correlate with increased use of air conditioning systems and outdoor water features during warmer months. Healthcare facilities face particular challenges due to vulnerable patient populations and complex water systems requiring specialized maintenance protocols. The disease's association with travel, particularly stays in hotels and cruise ships, highlights how modern lifestyle and tourism can facilitate exposure to contaminated environmental sources.
6. Whooping Cough - The Cyclical Respiratory Threat

Pertussis, commonly known as whooping cough, is caused by Bordetella pertussis bacteria and demonstrates cyclical epidemic patterns that reflect complex interactions between immunity, vaccination coverage, and bacterial evolution. The disease spreads through respiratory droplets produced during the characteristic paroxysmal coughing fits, with infected individuals most contagious during the early catarrhal stage when symptoms resemble a common cold. Waning immunity from both vaccination and natural infection creates periodic susceptibility in populations, leading to epidemic cycles every 3-5 years in many regions. Infants under six months face the highest mortality risk, as they are too young to be fully vaccinated and rely on maternal antibodies and community immunity for protection. School-age children and adolescents often serve as transmission bridges, carrying infection between households and communities due to their extensive social contact networks. The bacteria's evolution, including changes in virulence factors and vaccine antigen expression, has contributed to increased circulation despite high vaccination coverage in some populations. Household transmission rates are particularly high, with secondary attack rates reaching 80% among susceptible family members in close contact with infected individuals. Healthcare settings require careful management of suspected cases, as the disease can spread rapidly among patients and staff before diagnosis is confirmed. Seasonal patterns typically show increased transmission during late summer and fall months, coinciding with school reopening and increased indoor activities. The resurgence of pertussis in some developed countries despite vaccination programs highlights the ongoing challenges of maintaining population immunity against evolving pathogens.
7. Chickenpox and Shingles - The Dual-Phase Viral Challenge
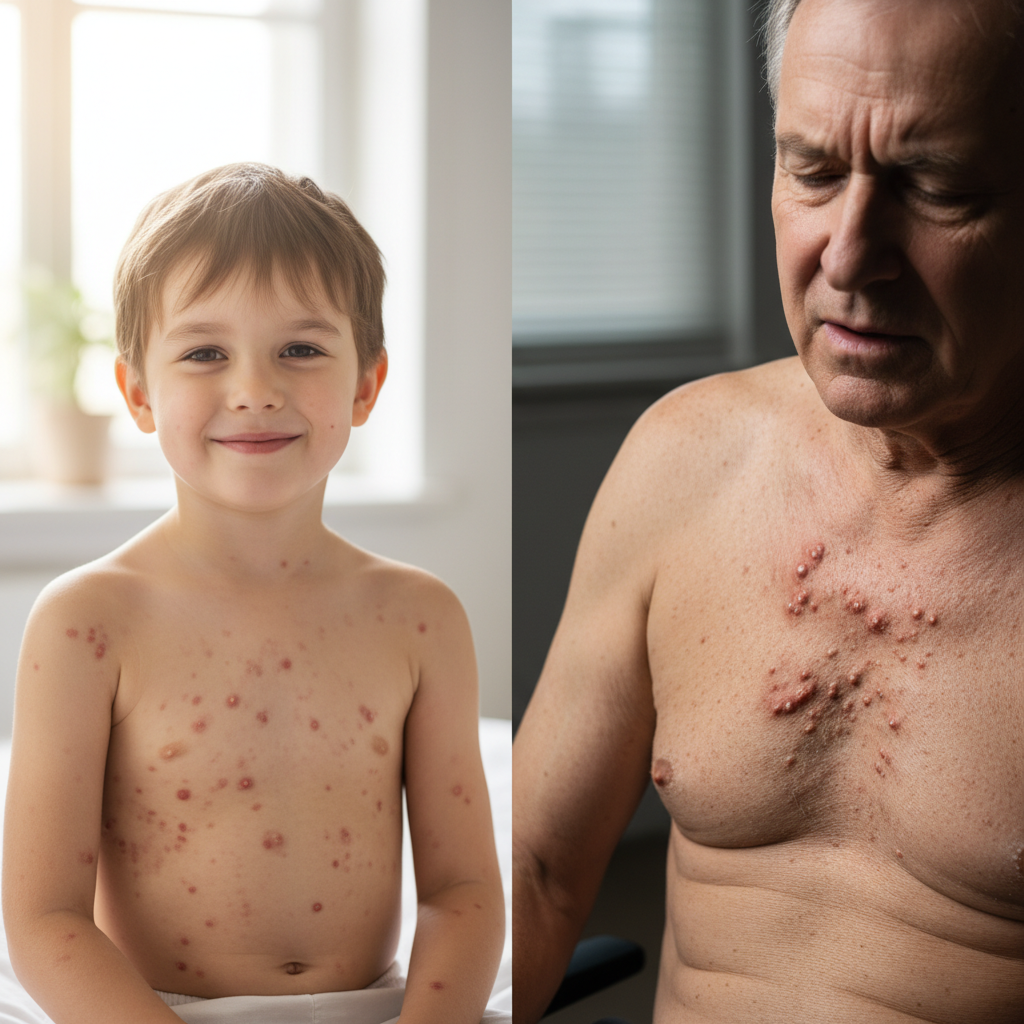
Varicella-zoster virus (VZV) presents a unique airborne transmission challenge through its dual manifestation as chickenpox (primary infection) and shingles (reactivation), creating ongoing transmission risks throughout an individual's lifetime. Chickenpox spreads extremely efficiently through respiratory droplets and aerosols, with the virus remaining viable in air for extended periods and capable of traveling significant distances through ventilation systems. The disease's high contagiosity, with attack rates approaching 90% in susceptible household contacts, makes outbreak control particularly challenging in schools and childcare facilities. Seasonal patterns typically show increased transmission during late winter and early spring in temperate climates, correlating with indoor crowding and environmental conditions favoring viral survival. Age-related susceptibility patterns show that while chickenpox primarily affects children, adult infections tend to be more severe, creating healthcare management challenges. Immunocompromised individuals face particular risks from both primary infection and reactivation, with disseminated disease potentially proving fatal without appropriate treatment. Healthcare settings require strict airborne precautions for both chickenpox and disseminated shingles cases, as nosocomial transmission can affect vulnerable patients and susceptible staff members. The virus's ability to remain dormant in nerve ganglia and reactivate as shingles creates ongoing transmission potential, particularly among elderly populations where reactivation rates increase significantly. Vaccination programs have dramatically reduced chickenpox incidence, but breakthrough infections can still occur and may present with atypical symptoms, complicating diagnosis and control efforts. International travel can facilitate virus spread between populations with different vaccination policies and natural immunity levels.
8. Aspergillosis - The Fungal Airborne Menace
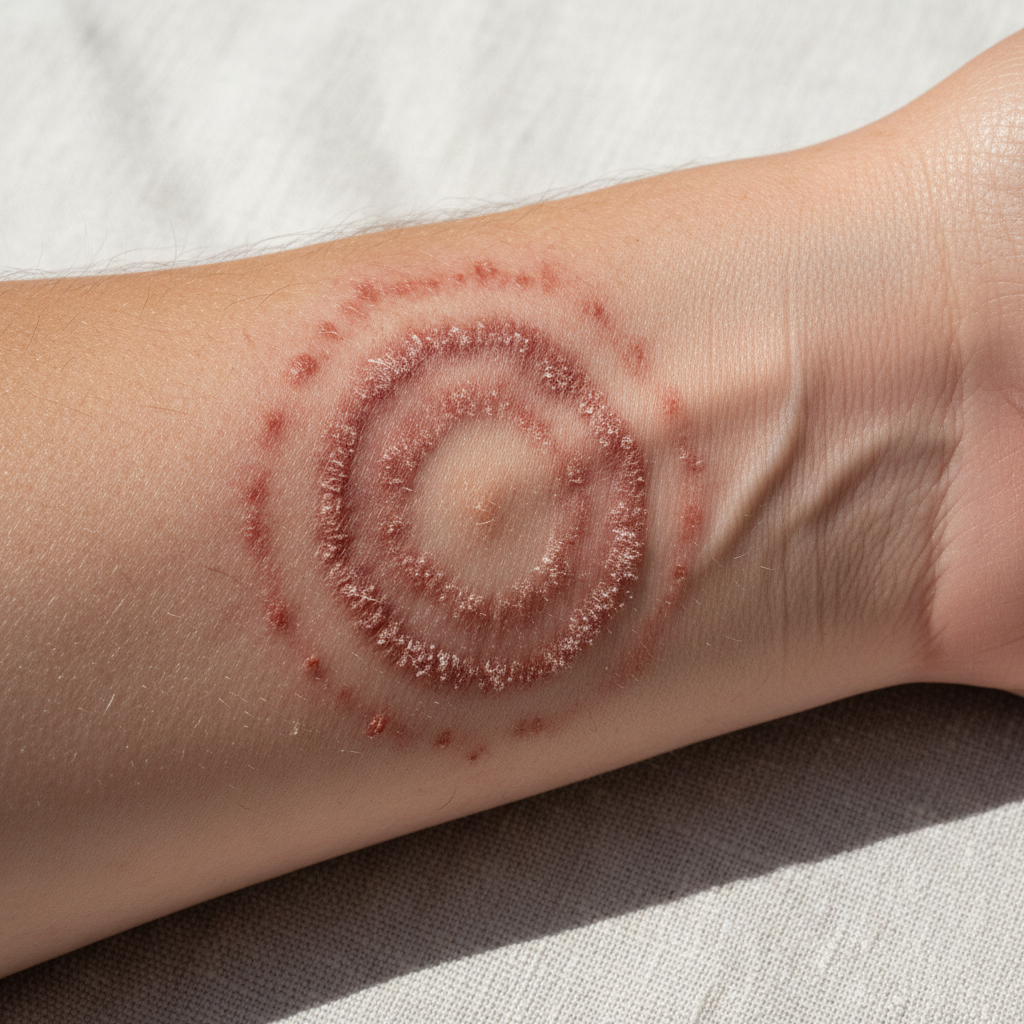
Aspergillosis represents a significant category of airborne fungal diseases caused by Aspergillus species, with transmission occurring through inhalation of ubiquitous environmental spores that become problematic under specific host and environmental conditions. Unlike bacterial or viral airborne diseases, Aspergillus spores are constantly present in outdoor and indoor environments, making exposure inevitable but infection dependent on individual susceptibility factors and spore concentration levels. Construction activities, renovation projects, and soil disturbance dramatically increase airborne spore concentrations, creating high-risk exposure scenarios particularly dangerous for immunocompromised individuals. Healthcare facilities face unique challenges in preventing aspergillosis, requiring specialized air filtration systems, positive pressure rooms, and strict environmental controls during construction or maintenance activities. Seasonal variations in outdoor spore counts, typically peaking during dry, windy conditions in late summer and fall, influence infection patterns and guide preventive measures for at-risk populations. Indoor environments can harbor Aspergillus growth in damp areas, ventilation systems, and organic materials, creating ongoing exposure risks that require environmental assessment and remediation. Immunocompromised patients, including those undergoing chemotherapy, organ transplant recipients, and individuals with chronic granulomatous disease, face life-threatening invasive infections with mortality rates exceeding 50% in some populations. Agricultural workers and individuals involved in composting or handling organic materials experience occupational exposure risks, particularly when protective equipment is inadequate. Climate change and urbanization patterns may alter environmental Aspergillus distribution and concentration, potentially affecting future infection patterns and geographic risk areas. The fungus's resistance to many antifungal agents and ability to form biofilms complicate treatment efforts and environmental control measures.
9. Anthrax - The Bioterrorism Concern

Pulmonary anthrax, caused by inhalation of Bacillus anthracis spores, represents both a natural occupational hazard and a potential bioterrorism threat, with transmission characteristics that differ significantly from other airborne pathogens. The disease does not spread person-to-person, instead requiring direct inhalation of spores that can remain viable in the environment for decades under appropriate conditions. Occupational exposure historically occurred among workers handling animal products, particularly wool, hides, and hair from infected animals, giving the disease its alternative name "woolsorter's disease." The spores' remarkable environmental stability and resistance to heat, cold, radiation, and chemical disinfectants make them particularly concerning from a biodefense perspective. Particle size plays a critical role in pathogenicity, with spores 1-5 micrometers in diameter most likely to reach the alveolar spaces where infection initiates. Industrial processes that create aerosols from contaminated materials pose the highest risk, requiring specialized ventilation systems and personal protective equipment for worker safety. The 2001 anthrax letter attacks demonstrated how small quantities of weaponized spores could cause widespread fear and disruption, highlighting vulnerabilities in postal and office building ventilation systems. Geographic factors influence natural exposure risks, with certain regions having higher rates of animal anthrax and corresponding human exposure potential. Laboratory safety protocols for handling B. anthracis require the highest biosafety levels due to the extreme infectivity of aerosolized spores. Environmental detection and decontamination following potential exposure events require sophisticated techniques and can be extremely costly and time-consuming, as demonstrated in the aftermath of the 2001 attacks.
10. Environmental and Architectural Factors in Disease Transmission

The built environment plays a crucial role in either facilitating or preventing airborne disease transmission, with architectural design, ventilation systems, and building maintenance practices serving as critical determinants of infection risk. Ventilation rates, measured in air changes per hour, directly impact pathogen concentration levels, with inadequate ventilation allowing infectious particles to accumulate and increase exposure risks for occupants. Building height and design influence air circulation patterns, with tall buildings often experiencing stack effects that can distribute contaminated air vertically between floors through elevator shafts and stairwells. Humidity levels significantly affect pathogen survival and transmission, with many viruses surviving longer in low humidity conditions while bacteria and fungi may thrive in higher humidity environments. Indoor air quality monitoring has become increasingly sophisticated, with carbon dioxide sensors serving as proxies for ventilation adequacy and potential infection risk in occupied spaces. HVAC system design and maintenance practices can either mitigate or exacerbate transmission risks, with proper filtration, UV disinfection, and regular maintenance reducing pathogen loads while poorly maintained systems can serve as amplification and distribution networks. Occupancy density and space utilization patterns influence contact rates and exposure duration, with crowded spaces facilitating rapid transmission even in well-ventilated environments. Natural ventilation through windows and doors can provide significant benefits in appropriate climates, often achieving higher air change rates than mechanical systems while reducing energy consumption. Building materials and surface treatments can influence pathogen survival, with some materials harboring microorganisms while others possess antimicrobial properties. The COVID-19 pandemic has accelerated adoption of building modifications including improved filtration, UV disinfection systems, and enhanced ventilation controls designed to reduce airborne transmission risks.
11. Climate Change and Future Airborne Disease Patterns

Climate change is fundamentally altering the landscape of airborne disease transmission through multiple interconnected mechanisms that affect pathogen survival, vector distribution, human behavior, and environmental conditions. Rising global temperatures are extending the geographic range and seasonal activity periods of many pathogens, potentially introducing airborne diseases to previously unaffected regions and populations. Changing precipitation patterns create new environmental niches for pathogen growth and aerosolization, with both drought and flooding conditions potentially increasing airborne disease risks through different mechanisms. Extreme weather events, including hurricanes, wildfires, and dust storms, can mobilize and distribute pathogens across vast distances, creating exposure risks far from original sources. Urban heat island effects concentrate climate impacts in densely populated areas, potentially creating hotspots for airborne disease transmission as people seek air-conditioned indoor environments with potentially inadequate ventilation. Agricultural changes driven by climate shifts may alter occupational exposure patterns to fungal and bacterial pathogens, particularly as farming practices adapt to new temperature and moisture regimes. Migration patterns influenced by climate change can introduce airborne pathogens to new populations and geographic areas, potentially overwhelming local healthcare systems unprepared for specific diseases. Air quality degradation from increased wildfire activity and changing weather patterns may compromise respiratory health and increase susceptibility to airborne infections across broad populations. Seasonal timing shifts in traditional disease patterns may disrupt established prevention and control programs, requiring adaptive management strategies and flexible response capabilities. The interaction between climate change and urbanization creates complex scenarios where multiple risk factors converge, potentially accelerating airborne disease transmission in ways that current models may not fully predict, emphasizing the need for integrated approaches to climate adaptation and public health preparedness.