10 Autoimmune Diseases That Vary in Prevalence Across Populations
Autoimmune diseases represent a fascinating intersection of genetics, environment, and population dynamics, creating a complex mosaic of prevalence patterns that vary dramatically across different ethnic groups, geographic regions, and populations worldwide. These conditions, where the immune system mistakenly attacks the body's own tissues, affect millions globally, yet their distribution is far from uniform. From the higher rates of multiple sclerosis in Northern European populations to the increased prevalence of systemic lupus erythematosus in African American women, these variations reveal intricate relationships between ancestry, environmental factors, and disease susceptibility. Understanding these population-specific patterns is crucial not only for healthcare providers and researchers but also for developing targeted prevention strategies and treatment approaches. The disparities in autoimmune disease prevalence across populations reflect a complex interplay of genetic predisposition, environmental triggers, socioeconomic factors, and healthcare access, making this field of study both challenging and essential for advancing global health equity.
1. Multiple Sclerosis - The Northern Latitude Phenomenon

Multiple sclerosis (MS) demonstrates one of the most striking examples of geographic and ethnic variation in autoimmune disease prevalence, with rates dramatically higher in populations of Northern European descent and in regions farther from the equator. This neurological condition, which affects the central nervous system by causing the immune system to attack myelin sheaths, shows a prevalence gradient that increases with latitude, particularly in the Northern Hemisphere. Scandinavian countries, Scotland, and Canada report some of the highest MS rates globally, with prevalence reaching up to 200 cases per 100,000 people in some regions. Conversely, populations in tropical and subtropical regions, including most of Africa, Asia, and parts of South America, show significantly lower rates. This pattern has led researchers to investigate the "latitude hypothesis," which suggests that reduced sunlight exposure and subsequent vitamin D deficiency may play a crucial role in MS development. Additionally, genetic factors are significant, with certain HLA alleles more common in Northern European populations being associated with increased MS risk. The disease affects women approximately three times more often than men across most populations, though this gender disparity varies slightly between ethnic groups. Recent migration studies have provided additional insights, showing that individuals who migrate from low-risk to high-risk regions during childhood may adopt the risk profile of their new environment, while adult migrants tend to retain the risk characteristics of their birthplace.
2. Systemic Lupus Erythematosus - Disproportionate Impact on Women of Color

Systemic lupus erythematosus (SLE) presents a stark example of how autoimmune diseases can disproportionately affect specific populations, with African American, Hispanic, Asian, and Native American women experiencing significantly higher rates and more severe disease manifestations compared to Caucasian populations. This multisystem autoimmune disease, characterized by the production of autoantibodies that attack various organs and tissues, affects approximately 1 in 537 young African American women compared to 1 in 2,000 young Caucasian women. The disparity extends beyond mere prevalence to include disease severity, with women of color more likely to develop lupus nephritis, neuropsychiatric complications, and cardiovascular manifestations. Hispanic and Asian populations also show elevated rates, though the specific prevalence varies among subgroups within these broad categories. Genetic studies have identified population-specific risk alleles, including variants in genes such as STAT4, IRF5, and PTPN22, which contribute to these disparities. Environmental factors, including socioeconomic status, access to healthcare, stress levels, and exposure to certain infections, may also play roles in the observed differences. The age of onset tends to be earlier in African American and Hispanic women, and these populations often experience more aggressive disease courses with higher mortality rates. Research has also revealed differences in autoantibody profiles between populations, with certain antibodies being more prevalent in specific ethnic groups, potentially influencing disease manifestations and treatment responses.
3. Type 1 Diabetes - The Scandinavian Paradox

Type 1 diabetes mellitus exhibits remarkable population-based variation, with Finland holding the unfortunate distinction of having the world's highest incidence rates, followed closely by other Scandinavian countries and Sardinia. This autoimmune condition, where the immune system destroys insulin-producing beta cells in the pancreas, shows a striking north-south gradient in Europe, with incidence rates decreasing as one moves toward the Mediterranean. Finland reports annual incidence rates exceeding 60 cases per 100,000 children under 15, while countries in Asia and Africa often report rates below 5 per 100,000. The reasons for this dramatic variation are multifactorial and include genetic susceptibility patterns, environmental triggers, and lifestyle factors. Populations with high frequencies of specific HLA alleles, particularly HLA-DR3 and HLA-DR4, show increased susceptibility, and these alleles are more common in Northern European populations. The hygiene hypothesis has been proposed to explain some of these differences, suggesting that reduced early-life exposure to pathogens in developed countries may contribute to autoimmune disease development. Interestingly, migration studies have shown that children from low-incidence populations who move to high-incidence countries may develop increased risk over time, while maintaining some protection compared to the native population. The seasonal pattern of diagnosis also varies by population, with many Northern European countries showing peak diagnoses in winter months, while this pattern is less pronounced in populations closer to the equator.
4. Rheumatoid Arthritis - Native American Vulnerability

Rheumatoid arthritis (RA) demonstrates significant population-based variations, with Native American populations, particularly certain tribes, experiencing some of the highest prevalence rates globally, while some Asian and African populations show relatively lower rates. This chronic inflammatory condition affecting joints and other organs shows particularly elevated rates among the Pima Indians of Arizona and the Chippewa tribe, with prevalence rates reaching 5-7% in some communities, compared to approximately 1% in the general U.S. population. The increased susceptibility in Native American populations has been linked to specific genetic factors, including a higher frequency of the shared epitope in HLA-DRB1 alleles and unique genetic variants that may have been selected for during population bottlenecks in ancestral history. European populations generally show moderate to high RA prevalence, with rates varying from 0.5% to 1.5% across different countries. Interestingly, some sub-Saharan African populations have historically shown lower RA rates, though this may be changing with urbanization and lifestyle modifications. The disease also shows gender disparities that vary across populations, with women generally affected 2-3 times more often than men, though this ratio can vary between ethnic groups. Environmental factors, including smoking, diet, and exposure to certain infections, interact differently with genetic backgrounds across populations, contributing to the observed variations. Recent research has also highlighted differences in disease severity and progression patterns between populations, with some groups experiencing more aggressive joint destruction while others may have more systemic manifestations.
5. Inflammatory Bowel Disease - The Western World Burden
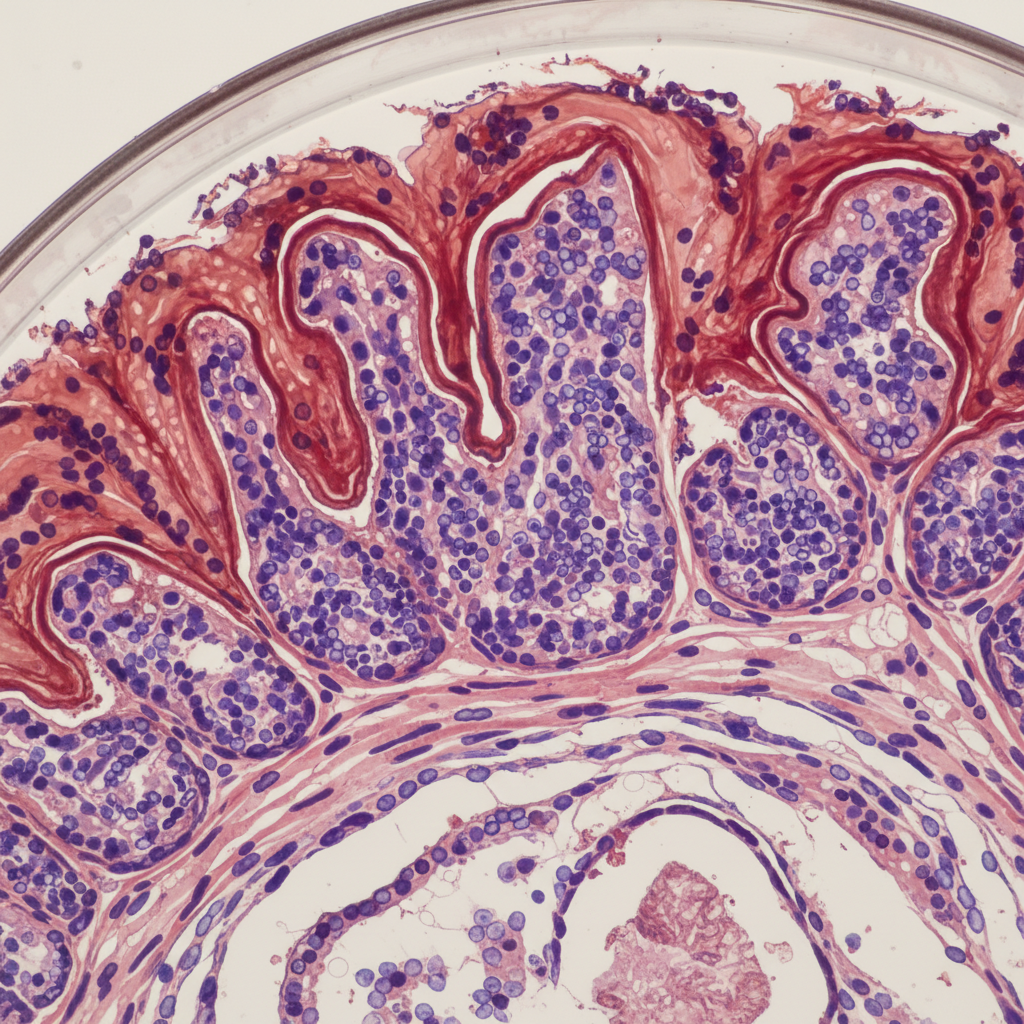
Inflammatory bowel disease (IBD), encompassing Crohn's disease and ulcerative colitis, shows a distinctive pattern of higher prevalence in developed Western countries and among populations of European descent, while remaining relatively uncommon in many developing regions of Asia, Africa, and South America. This chronic inflammatory condition of the gastrointestinal tract affects approximately 1.5 million Americans and 2.5 million Europeans, with the highest rates observed in Northern European countries, North America, and Australia. Ashkenazi Jewish populations demonstrate particularly elevated rates, with some studies showing 2-4 times higher prevalence compared to non-Jewish populations in the same geographic areas. The urban-rural divide is pronounced in IBD, with urban populations consistently showing higher rates, suggesting that lifestyle factors associated with westernization play important roles. However, this pattern is rapidly changing as developing countries undergo economic transition, with rising IBD rates now being reported in Asia, the Middle East, and parts of South America. Genetic studies have identified over 200 susceptibility loci for IBD, with some variants showing population-specific effects. For instance, certain NOD2 mutations are common in European IBD patients but rare in Asian populations, while other genetic variants show opposite patterns. The hygiene hypothesis is particularly relevant to IBD, as reduced early-life microbial exposure in developed countries may contribute to immune system dysfunction. Environmental factors including diet (particularly Western dietary patterns), antibiotic use, smoking, and stress levels all contribute to the observed population differences in IBD prevalence and may explain the increasing rates in transitioning societies.
6. Celiac Disease - European Ancestry and Global Spread

Celiac disease exhibits a strong association with European ancestry, particularly affecting populations from Ireland, Italy, and other regions where wheat consumption has been historically prevalent, while remaining relatively uncommon in East Asian and sub-Saharan African populations. This autoimmune condition triggered by gluten consumption affects approximately 1% of the global population, but prevalence rates vary dramatically across different ethnic groups and geographic regions. Irish populations show some of the highest rates globally, with prevalence reaching 1 in 100 individuals, while Scandinavian countries also report elevated rates. The disease requires specific genetic predisposition, with nearly all patients carrying HLA-DQ2 or HLA-DQ8 alleles, which are much more common in populations of European descent. Interestingly, North African populations, particularly those from the Sahara region, also show relatively high rates of celiac disease, likely due to historical genetic mixing with European populations and long-standing wheat cultivation. The prevalence in Middle Eastern populations varies considerably, with some groups showing rates similar to Europeans while others have much lower prevalence. Migration patterns have spread celiac disease globally, with second and third-generation immigrants from high-prevalence regions maintaining elevated risk even when living in areas where the disease was historically rare. Recent studies have also revealed that the clinical presentation of celiac disease can vary between populations, with some groups more likely to present with classical gastrointestinal symptoms while others may have predominantly extraintestinal manifestations. The increasing global availability of wheat-based foods and changing dietary patterns are leading to rising celiac disease diagnoses in previously low-prevalence populations, though genetic susceptibility remains the primary determining factor.
7. Sjögren's Syndrome - Mediterranean and Scandinavian Clusters

Sjögren's syndrome, an autoimmune condition primarily affecting the salivary and lacrimal glands leading to dry mouth and dry eyes, shows interesting population-based clustering with particularly high rates observed in Mediterranean countries and Scandinavian regions, while being less common in many Asian and African populations. This condition, which affects approximately 0.5-1% of the global population, demonstrates a strong female predominance across all populations, with women being 9-10 times more likely to be affected than men. Greek and Italian populations have reported some of the highest prevalence rates, with certain regions showing rates exceeding 3% in older women. Scandinavian countries, particularly Sweden and Norway, also report elevated rates, suggesting possible genetic or environmental factors common to these regions. The disease shows interesting ethnic variations within multi-ethnic countries, with studies in the United States indicating higher rates among Caucasian women compared to African American or Hispanic women, though these differences may be influenced by healthcare access and diagnostic practices. Genetic studies have identified several population-specific risk alleles, including variants in genes such as IRF5, STAT4, and BLK, which show different frequencies across ethnic groups. Environmental factors, including viral infections (particularly Epstein-Barr virus), hormonal influences, and possibly dietary factors, may interact differently with genetic backgrounds across populations. The clinical presentation can also vary between populations, with some groups more likely to develop systemic complications including lymphoma, while others may have predominantly glandular manifestations. Recent research has highlighted differences in autoantibody profiles between populations, which may influence disease progression and treatment responses.
8. Vitiligo - Global Distribution with Population-Specific Patterns
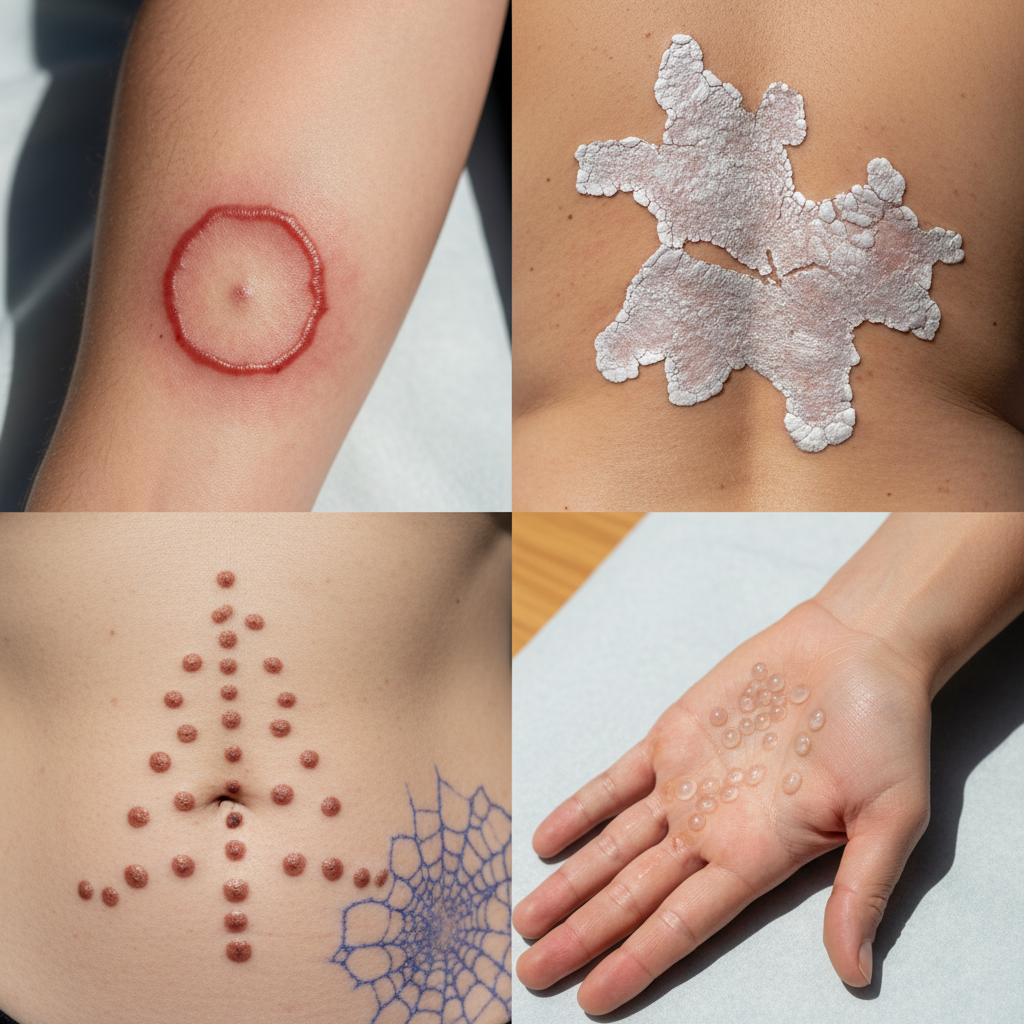
Vitiligo, an autoimmune condition causing depigmentation of the skin, affects approximately 0.5-2% of the global population but shows significant variation in prevalence, clinical presentation, and psychosocial impact across different ethnic groups and geographic regions. While the condition occurs in all populations, it tends to be more noticeable and potentially more psychologically distressing in individuals with darker skin tones, leading to possible underreporting in lighter-skinned populations and overreporting in darker-skinned groups. Indian populations, particularly those from certain regions of India, report some of the highest prevalence rates globally, with some studies indicating rates up to 8% in certain communities. The condition also shows relatively high prevalence in parts of Mexico, Turkey, and some Mediterranean countries. Genetic studies have revealed population-specific susceptibility alleles, with different genes playing varying roles across ethnic groups. For instance, certain variants in the TYR gene are more important in European populations, while other genetic factors may be more relevant in Asian or African populations. The clinical presentation of vitiligo can vary significantly between populations, with some groups more likely to develop segmental vitiligo while others predominantly develop non-segmental forms. Age of onset also varies, with some populations showing earlier onset patterns. Environmental triggers, including stress, trauma, and chemical exposure, may have different impacts across populations due to varying occupational exposures and lifestyle factors. The psychosocial impact of vitiligo varies dramatically across cultures, with some societies showing greater stigmatization of visible skin conditions, potentially affecting treatment-seeking behavior and quality of life measures.
9. Hashimoto's Thyroiditis - Iodine, Genetics, and Geographic Clustering
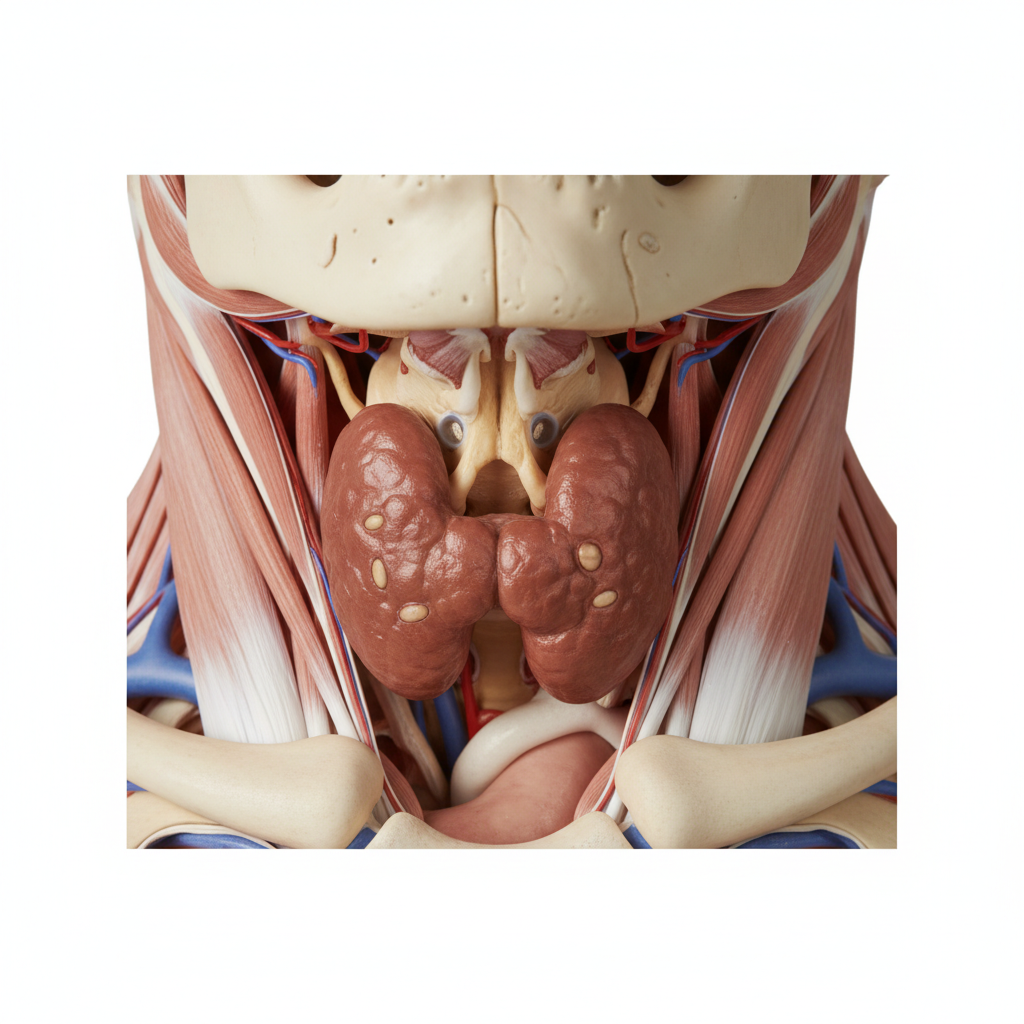
Hashimoto's thyroiditis, the most common cause of hypothyroidism in iodine-sufficient areas, demonstrates significant population-based variation influenced by genetic factors, iodine intake, and environmental conditions. This autoimmune condition affecting the thyroid gland shows particularly high prevalence in populations with adequate or excessive iodine intake, including many developed countries, while being less common in iodine-deficient regions. Japanese populations have historically shown some of the highest rates of Hashimoto's thyroiditis, likely related to their traditionally high iodine intake from seaweed consumption, with prevalence rates reaching 10-15% in some studies of older women. Scandinavian countries also report elevated rates, possibly due to both genetic factors and iodine supplementation programs. The condition shows a strong female predominance across all populations, with women being 5-10 times more likely to be affected, though the exact ratio varies between ethnic groups. Genetic studies have identified population-specific risk alleles, including variants in HLA genes, CTLA-4, and PTPN22, which show different frequencies across ethnic groups. Ashkenazi Jewish populations demonstrate elevated rates compared to other groups in the same geographic areas, suggesting genetic founder effects. Environmental factors play crucial roles, with iodine intake being particularly important – populations transitioning from iodine deficiency to sufficiency often show temporary increases in autoimmune thyroid disease. Selenium deficiency, which is more common in certain geographic regions, may also contribute to population differences in Hashimoto's prevalence and severity. The clinical presentation can vary between populations, with some groups more likely to develop goiter while others may present primarily with hypothyroid symptoms.
10. Psoriasis - Climate, Genetics, and Cultural Factors

Psoriasis, a chronic autoimmune skin condition, exhibits remarkable population-based variation with higher prevalence in Northern European populations and lower rates in many Asian, African, and Native American groups, reflecting complex interactions between genetic susceptibility, environmental triggers, and cultural factors. This condition affects approximately 2-3% of the global population but shows dramatic geographic clustering, with Scandinavian countries reporting some of the highest rates, reaching up to 11% in certain regions of Norway. The Faroe Islands hold the distinction of having the world's highest reported psoriasis prevalence, with rates exceeding 2.8% of the population. Conversely, many sub-Saharan African populations, East Asian groups, and indigenous populations of the Americas show significantly lower rates, often below 0.5%. Genetic studies have identified over 60 susceptibility loci for psoriasis, with the HLA-C*06:02 allele being particularly important in European populations but less relevant in many non-European groups. Different populations may have distinct genetic risk profiles, with some variants being protective in certain ethnic groups while being risk factors in others. Environmental factors contribute significantly to population differences, with climate playing a crucial role – UV exposure generally improves psoriasis, which may partly explain the lower prevalence in sunny, tropical regions. However, this relationship is complex, as some sunny regions still show elevated rates. Cultural factors, including clothing practices, dietary habits, and stress levels, also contribute to population differences. The clinical presentation of psoriasis can vary between populations, with some groups more likely to develop certain subtypes or experience different patterns of joint involvement in psoriatic arthritis.
11. Implications for Global Health and Future Research

The striking variations in autoimmune disease prevalence across populations underscore the complex interplay between genetics, environment, and culture in determining disease susceptibility and outcomes. These patterns reveal that autoimmune diseases are not merely random occurrences but rather reflect the evolutionary history, genetic diversity, and environmental exposures of different human populations. Understanding these variations has profound implications for global health policy, clinical practice, and research priorities. Healthcare systems must recognize that diagnostic criteria, treatment protocols, and prevention strategies developed in one population may not be directly applicable to others, necessitating population-specific approaches to autoimmune disease management. The observed disparities also highlight health equity issues, as some populations bear disproportionate burdens of certain autoimmune conditions while having limited access to specialized care or research attention. Future research must prioritize studying underrepresented populations, developing culturally appropriate interventions, and investigating how changing global environments – including urbanization, dietary transitions, and climate change – may alter traditional patterns of autoimmune disease distribution. As populations become increasingly mobile and intermixed, understanding these baseline patterns becomes even more critical for predicting future disease trends and developing effective prevention strategies. The field of precision medicine holds particular promise for autoimmune diseases, as population-specific genetic and environmental risk factors could inform personalized prevention and treatment approaches, ultimately leading to better outcomes for