8 Neglected Tropical Diseases Receiving Increased Global Attention
Neglected tropical diseases (NTDs) represent one of the most profound health inequities of our time, affecting over 1.7 billion people worldwide, predominantly in impoverished communities across Africa, Asia, and Latin America. These diseases, which include conditions like lymphatic filariasis, onchocerciasis, schistosomiasis, and Chagas disease, have historically received minimal attention from the global health community despite their devastating impact on human development and economic productivity. The term "neglected" itself reflects decades of insufficient research funding, limited pharmaceutical development, and inadequate public health infrastructure dedicated to combating these conditions. However, a remarkable transformation has begun to unfold over the past decade, driven by unprecedented collaboration between international organizations, governments, pharmaceutical companies, and non-governmental organizations. The World Health Organization's ambitious roadmap for NTDs, coupled with increased funding from entities like the Bill & Melinda Gates Foundation and innovative partnerships such as the London Declaration on NTDs, has catalyzed a new era of hope and progress. This renewed focus represents not merely a medical intervention but a comprehensive approach to breaking the vicious cycle of poverty and disease that has trapped entire communities for generations.
1. Lymphatic Filariasis - The Hidden Epidemic of Swollen Limbs
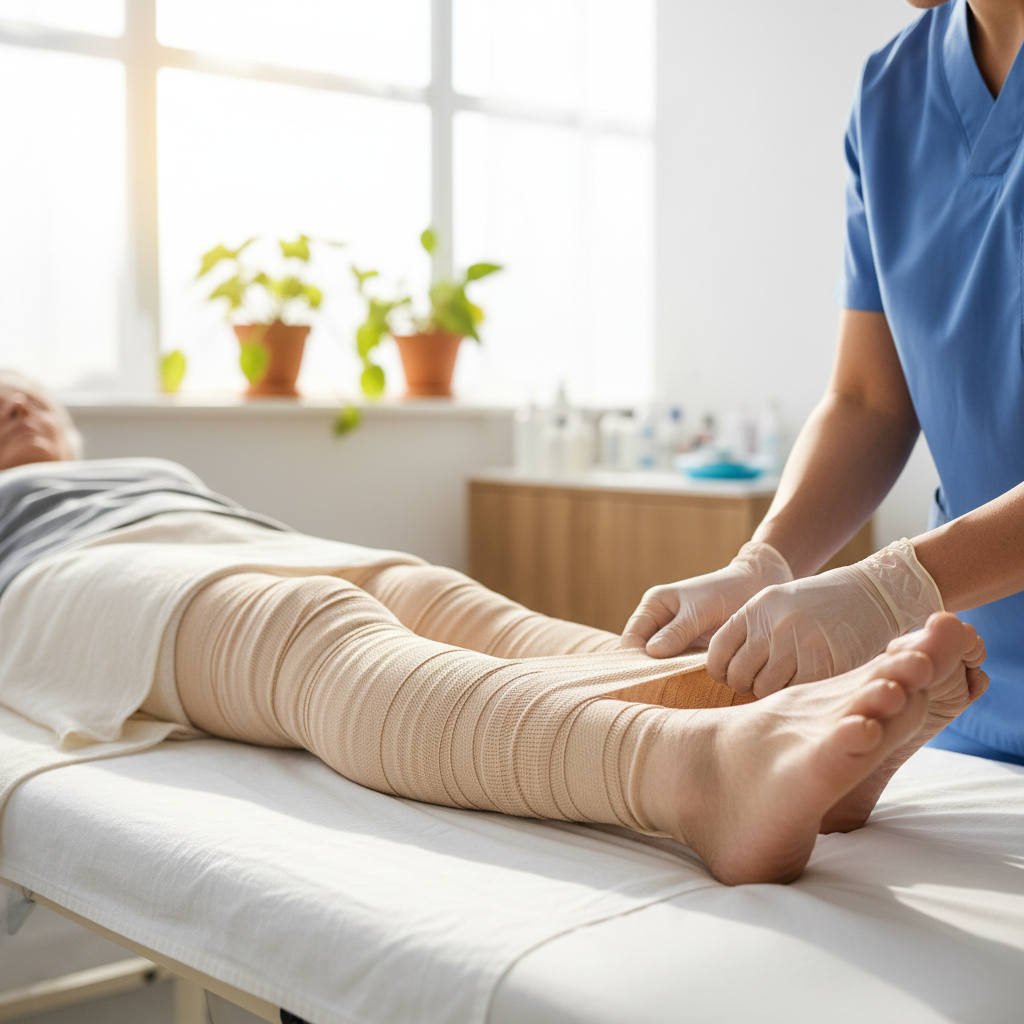
Lymphatic filariasis, commonly known as elephantiasis, stands as one of the most visually striking and socially stigmatizing neglected tropical diseases, affecting over 120 million people globally with another 856 million at risk of infection. Caused by parasitic worms transmitted through mosquito bites, this disease progressively damages the lymphatic system, leading to severe swelling of limbs and genitals that can render individuals unable to work or participate fully in society. The increased global attention toward lymphatic filariasis has been particularly remarkable, with the Global Programme to Eliminate Lymphatic Filariasis achieving unprecedented success through mass drug administration campaigns. Countries like Egypt, Cambodia, and the Maldives have successfully eliminated the disease as a public health problem, demonstrating that with sustained commitment and resources, even the most entrenched NTDs can be conquered. The strategy involves annual distribution of preventive medications to entire at-risk populations, combined with improved sanitation and vector control measures. Recent innovations include the development of new diagnostic tools that can detect infection even in asymptomatic individuals, enabling more targeted interventions. The economic impact of these efforts has been substantial, with every dollar invested in elimination programs yielding an estimated $24 in economic benefits through reduced healthcare costs and increased productivity.
2. Onchocerciasis - River Blindness No Longer Inevitable

Onchocerciasis, or river blindness, has historically been one of the leading infectious causes of blindness worldwide, affecting approximately 21 million people, with 90% of cases concentrated in sub-Saharan Africa. The disease is caused by the parasitic worm Onchocerca volvulus, transmitted through the bites of infected blackflies that breed in fast-flowing rivers, hence the name "river blindness." The transformation in addressing this disease began with the groundbreaking Onchocerciasis Control Programme in West Africa, launched in 1974, which demonstrated that large-scale elimination was possible through sustained intervention. The game-changer came with Merck & Co.'s decision to donate ivermectin (Mectizan) indefinitely, creating one of the most successful public-private partnerships in global health history. Today, the African Programme for Onchocerciasis Control continues this legacy, with several countries achieving elimination of transmission. Colombia became the first country in the Americas to be verified as free from onchocerciasis transmission in 2013, followed by Ecuador, Mexico, and Guatemala. The increased attention has also spurred research into alternative treatment strategies, including the development of new drugs targeting adult worms rather than just microfilariae, potentially shortening treatment duration from decades to years. Community-directed treatment programs have empowered local populations to take ownership of their health outcomes, creating sustainable models for disease control that extend beyond onchocerciasis.
3. Schistosomiasis - Ancient Parasite, Modern Solutions

Schistosomiasis, one of humanity's oldest documented diseases with evidence found in ancient Egyptian mummies, continues to plague over 240 million people worldwide, making it the second most socioeconomically devastating parasitic disease after malaria. Caused by parasitic flatworms that penetrate human skin during contact with contaminated freshwater, schistosomiasis primarily affects children and young adults in rural communities where access to clean water and sanitation remains limited. The renewed global focus on this disease has led to remarkable progress in treatment accessibility, with the World Health Organization facilitating the donation of over 100 million praziquantel tablets annually for school-age children in endemic countries. Recent years have witnessed innovative approaches to disease control, including the development of new formulations of praziquantel suitable for preschool children, who were previously unable to receive treatment due to the lack of appropriate pediatric formulations. Environmental management strategies have gained prominence, focusing on snail control and improved water, sanitation, and hygiene (WASH) infrastructure to interrupt transmission cycles. Countries like Morocco and Egypt have made significant strides toward elimination, while Brazil has successfully controlled the disease in several states. The integration of schistosomiasis control with other health programs, particularly those targeting soil-transmitted helminths, has created synergies that maximize resource utilization and improve overall health outcomes in affected communities.
4. Chagas Disease - The Silent Killer Gains a Voice

Chagas disease, often called the "silent killer" due to its asymptomatic chronic phase that can last decades before manifesting fatal cardiac complications, affects an estimated 6-7 million people worldwide, primarily in Latin America. Caused by the parasite Trypanosoma cruzi and traditionally transmitted through triatomine bugs known as "kissing bugs," this disease has historically received minimal attention despite being responsible for more deaths in Latin America than any other parasitic disease. The increased global focus on Chagas disease has been driven partly by its emergence in non-endemic countries through migration, blood transfusion, and organ transplantation, making it a truly global health concern. Innovative vector control strategies have shown remarkable success, with several countries achieving significant reductions in transmission through improved housing, insecticide application, and community education programs. The Southern Cone Initiative, launched in 1991, has been particularly successful, with Uruguay, Chile, and Brazil achieving interruption of transmission by the main vector species. Recent pharmaceutical developments have brought new hope, with simplified treatment regimens and pediatric formulations making treatment more accessible and tolerable. The integration of Chagas disease screening into routine healthcare systems, particularly for pregnant women and blood donors, has become a priority in many countries. Additionally, the development of rapid diagnostic tests has revolutionized case detection in remote areas where laboratory infrastructure is limited.
5. Soil-Transmitted Helminths - Worms That Steal Childhood

Soil-transmitted helminths, including roundworm, whipworm, and hookworm, represent the most prevalent neglected tropical diseases, infecting over 1.5 billion people globally, with children bearing the heaviest burden. These parasitic worms, transmitted through contaminated soil, rob children of their potential by causing malnutrition, anemia, and cognitive impairment that can persist throughout their lives. The increased attention to these infections has led to one of the largest public health interventions in history, with school-based deworming programs now reaching over 600 million children annually. The evidence base supporting mass deworming has grown substantially, with studies demonstrating not only immediate health benefits but also long-term improvements in educational attainment, income, and quality of life. Countries like Rwanda and Burundi have achieved remarkable coverage rates exceeding 95% of school-age children, while India's National Deworming Day has become the world's largest deworming program, treating over 260 million children annually. Innovation in program delivery has included the integration of deworming with other school health interventions, creating comprehensive packages that address multiple health needs simultaneously. The development of new drug formulations, including chewable tablets and dispersible formulations, has improved treatment acceptability among young children. Recent research has also highlighted the importance of combining deworming with water, sanitation, and hygiene interventions to achieve sustained reductions in infection rates and prevent reinfection.
6. Trachoma - Blinding Disease Meets Surgical Innovation
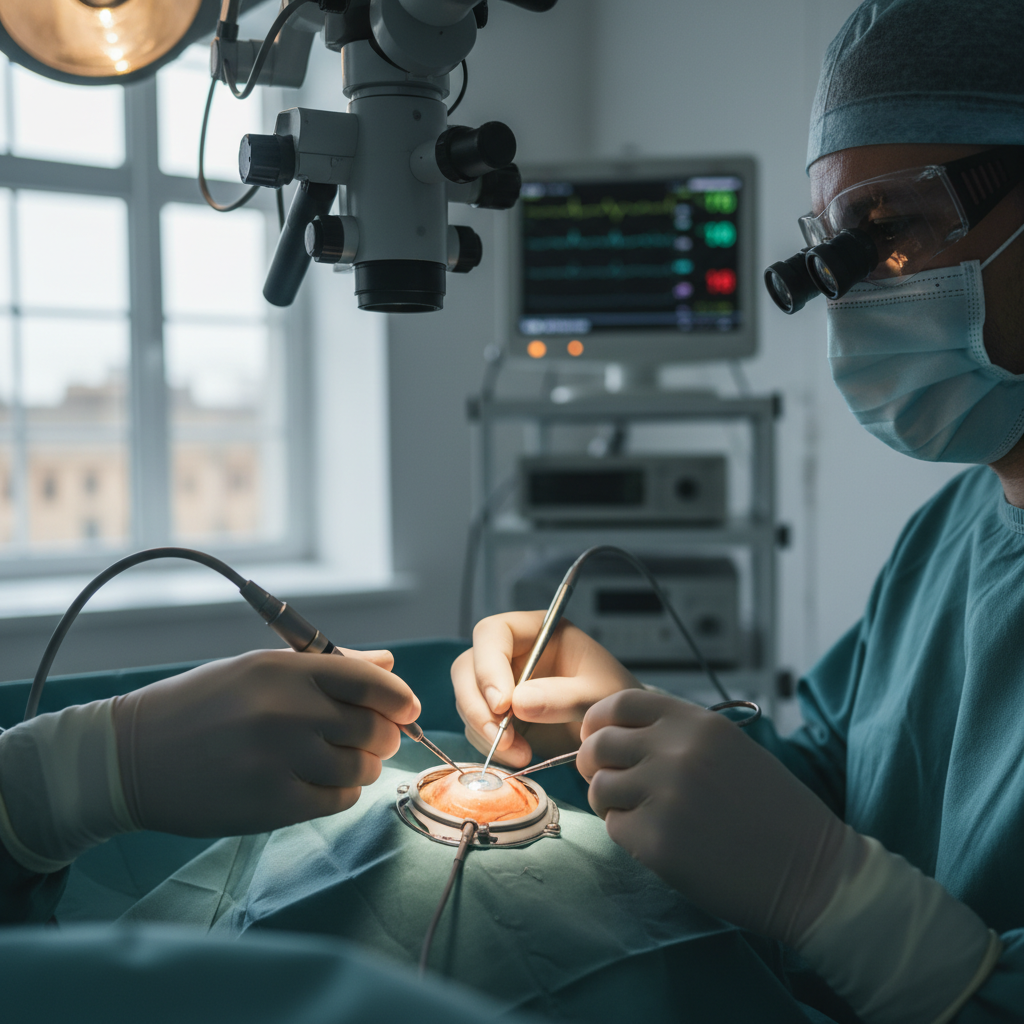
Trachoma, the leading infectious cause of blindness worldwide, affects over 136 million people in 44 countries, with the majority of cases concentrated in remote, impoverished communities across Africa, Asia, and Australia. This bacterial infection, caused by Chlamydia trachomatis, creates a cycle of repeated infections that eventually lead to scarring of the inner eyelid, causing the eyelashes to turn inward and scratch the cornea, ultimately resulting in irreversible blindness. The transformation in trachoma control has been driven by the WHO's SAFE strategy (Surgery, Antibiotics, Facial cleanliness, and Environmental improvement), which provides a comprehensive framework for elimination. The increased global attention has led to remarkable progress, with 11 countries successfully eliminating trachoma as a public health problem since 2016, including Ghana, Gambia, and Nepal. Surgical interventions for trichiasis (inward-turning eyelashes) have been revolutionized through training programs that have created a cadre of local surgeons capable of performing sight-saving operations in remote communities. The mass distribution of azithromycin, donated by Pfizer through the International Trachoma Initiative, has reached over 200 million people annually, dramatically reducing infection rates in endemic communities. Innovative approaches to facial cleanliness promotion and environmental improvement have addressed the root causes of transmission, with programs focusing on water access, latrine construction, and hygiene education. Recent technological advances include the development of smartphone-based diagnostic tools and artificial intelligence algorithms that can detect trachoma in field settings, potentially revolutionizing surveillance and case management.
7. Dengue and Vector Control - Urban Epidemic Meets Innovation

Dengue fever, while not traditionally classified among the most neglected tropical diseases, has gained unprecedented attention as urbanization and climate change have expanded its reach to affect over 390 million people annually across more than 100 countries. Transmitted by Aedes aegypti mosquitoes, dengue represents the fastest-spreading vector-borne disease globally, with incidence increasing eightfold over the past two decades. The increased focus on dengue has catalyzed innovative vector control strategies that extend beyond traditional approaches, including the release of genetically modified mosquitoes and Wolbachia-infected mosquitoes that reduce viral transmission. The World Mosquito Program has conducted groundbreaking field trials demonstrating that Wolbachia-infected mosquitoes can reduce dengue transmission by up to 77% in randomized controlled trials. Community-based vector control programs have proven highly effective, with countries like Singapore and Vietnam achieving significant reductions in mosquito breeding sites through sustained community engagement and education. The development of the first dengue vaccine, Dengvaxia, while facing initial challenges, has provided valuable lessons for future vaccine development and highlighted the importance of understanding local epidemiology before implementation. Recent innovations include the use of artificial intelligence and satellite imagery to predict dengue outbreaks, enabling proactive rather than reactive public health responses. The integration of dengue control with other vector-borne disease programs, particularly those targeting Zika and chikungunya, has created synergies that maximize the impact of limited resources while addressing multiple health threats simultaneously.
8. Human African Trypanosomiasis - Sleeping Sickness Awakens Hope

Human African trypanosomiasis, commonly known as sleeping sickness, has experienced one of the most dramatic transformations among neglected tropical diseases, declining from over 300,000 estimated cases in the 1990s to fewer than 1,000 reported cases in 2019. This vector-borne disease, transmitted by tsetse flies and caused by Trypanosoma brucei parasites, has historically devastated rural communities across sub-Saharan Africa, causing neurological damage and death if left untreated. The remarkable progress has been achieved through sustained political commitment, improved surveillance systems, and innovative public-private partnerships that have brought new diagnostic tools and treatments to remote endemic areas. The development of rapid diagnostic tests has revolutionized case detection, enabling healthcare workers in remote areas to diagnose the disease quickly and accurately without sophisticated laboratory infrastructure. Treatment has been transformed by the introduction of fexinidazole, an oral medication that can treat both stages of the disease caused by T. b. gambiense, replacing complex and dangerous treatment regimens that required hospitalization and intravenous administration. The WHO has set an ambitious target of eliminating sleeping sickness as a public health problem by 2030, and current trends suggest this goal is achievable. Vector control strategies have evolved to include innovative approaches such as tiny targets (insecticide-treated screens and traps) that specifically target tsetse flies while minimizing environmental impact. The success in controlling sleeping sickness has provided valuable lessons for addressing other vector-borne diseases and demonstrates that even the most challenging neglected tropical diseases can be brought under control with sustained effort and innovation.
9. The Road Ahead - Sustainable Elimination and Global Health Security

The unprecedented progress against neglected tropical diseases over the past decade has demonstrated that with sustained political commitment, adequate funding, and innovative partnerships, even the most entrenched health challenges can be overcome. However, the journey toward elimination and eventual eradication requires continued vigilance and adaptation to emerging challenges, including climate change, urbanization, population displacement, and the ongoing impacts of the COVID-19 pandemic on health systems worldwide. The integration of NTD programs with broader health system strengthening initiatives has emerged as a critical strategy for ensuring sustainability and maximizing impact. Countries that have successfully eliminated specific diseases have provided valuable blueprints for others, demonstrating the importance of strong surveillance systems, community engagement, and cross-border collaboration. The development of new tools and technologies, including improved diagnostics, simplified treatment regimens, and innovative vector control methods, continues to expand the arsenal available for disease control and elimination. Perhaps most importantly, the focus on neglected tropical diseases has highlighted the fundamental importance of addressing social determinants of health, including poverty, inadequate housing, limited access to clean water and sanitation, and weak health systems. The COVID-19 pandemic has underscored the interconnectedness of global health security and the importance of maintaining strong surveillance and response systems for all infectious diseases. As we look toward the future, the lessons learned from NTD control programs will be invaluable for addressing emerging health threats and achieving the Sustainable Development Goals. The transformation of neglected tropical diseases from forgotten ailments to global health priorities represents one of the most significant public health achievements of our time and provides hope that health equity can be achieved for all people, regardless of where they live or their economic circumstances.