8 Drug Allergy Types and How Reactions Differ from Side Effects
Drug allergies and side effects represent two fundamentally different physiological responses to medications, yet they are frequently confused by patients and even healthcare providers. A drug allergy is an immune system-mediated reaction that occurs when the body's immune system mistakenly identifies a medication as a harmful foreign substance, triggering an inflammatory response that can range from mild skin reactions to life-threatening anaphylaxis. In contrast, side effects are predictable, dose-dependent reactions that occur due to the medication's pharmacological properties and affect the body's normal physiological processes without involving the immune system. Understanding this distinction is crucial for proper medical management, as allergic reactions require immediate discontinuation of the offending medication and potential emergency treatment, while side effects may be manageable through dose adjustments or supportive care. The prevalence of true drug allergies is estimated at only 5-10% of all adverse drug reactions, making accurate identification essential for optimal patient care. This comprehensive exploration will examine eight distinct types of drug allergies, their unique characteristics, diagnostic approaches, and how they fundamentally differ from common medication side effects, providing healthcare professionals and patients with the knowledge necessary to recognize, prevent, and appropriately manage these potentially serious reactions.
1. Type I Hypersensitivity Reactions - The Immediate and Dangerous Response

Type I hypersensitivity reactions, also known as immediate hypersensitivity or IgE-mediated reactions, represent the most severe and rapidly occurring form of drug allergies. These reactions typically manifest within minutes to one hour after drug exposure and are mediated by immunoglobulin E (IgE) antibodies that have been previously formed against the specific medication or its metabolites. When the drug is reintroduced, it cross-links with IgE antibodies bound to mast cells and basophils, causing rapid degranulation and release of inflammatory mediators including histamine, leukotrienes, and prostaglandins. Clinical manifestations can range from localized urticaria and angioedema to systemic anaphylaxis, characterized by cardiovascular collapse, severe bronchospasm, and potentially fatal shock. Common culprits include penicillins, cephalosporins, aspirin, and certain chemotherapy agents. The severity and rapid onset of Type I reactions distinguish them clearly from side effects, which typically develop gradually and are dose-related. Diagnosis often relies on clinical history, skin testing, and measurement of drug-specific IgE levels, while management requires immediate discontinuation of the offending agent and emergency treatment with epinephrine, antihistamines, and corticosteroids for severe reactions.
2. Type II Cytotoxic Reactions - When Antibodies Attack Drug-Modified Cells
Type II hypersensitivity reactions, or cytotoxic reactions, occur when IgG or IgM antibodies bind to drug-modified cell surfaces, leading to complement activation and subsequent cell destruction through various mechanisms including complement-mediated lysis, antibody-dependent cellular cytotoxicity, and phagocytosis. These reactions typically develop over days to weeks after drug initiation and primarily affect blood cells, resulting in conditions such as drug-induced hemolytic anemia, thrombocytopenia, or neutropenia. The mechanism involves either the drug binding directly to cell surface proteins, forming a hapten-carrier complex, or the drug inducing conformational changes in cell surface antigens that make them appear foreign to the immune system. Classic examples include heparin-induced thrombocytopenia, where antibodies form against the heparin-platelet factor 4 complex, and quinidine-induced thrombocytopenia, where the drug binds to platelet glycoproteins. Unlike typical side effects that affect organ function through pharmacological mechanisms, Type II reactions specifically target cellular components for destruction, leading to cytopenias that can be life-threatening if severe. Laboratory diagnosis involves detecting drug-dependent antibodies through specialized assays, and treatment requires immediate drug discontinuation, supportive care for cytopenias, and sometimes immunosuppressive therapy in severe cases.
3. Type III Immune Complex Reactions - The Inflammatory Cascade
Type III hypersensitivity reactions involve the formation of immune complexes between drugs or their metabolites and circulating antibodies, typically IgG, which then deposit in tissues and activate complement, leading to inflammatory damage. These reactions usually develop 1-3 weeks after drug initiation and are characterized by serum sickness-like syndrome, featuring fever, arthralgia, lymphadenopathy, and skin rashes. The pathophysiology involves the formation of small immune complexes that circulate and deposit in blood vessel walls, joints, kidneys, and skin, where they activate complement and attract neutrophils, leading to tissue inflammation and damage. Drugs commonly associated with Type III reactions include sulfonamides, penicillins, and certain biologics. The clinical presentation often includes vasculitis, glomerulonephritis, and arthritis, which can be distinguished from drug side effects by the presence of immune complex deposition and complement consumption. Laboratory findings typically show decreased complement levels (C3, C4), elevated erythrocyte sedimentation rate, and sometimes circulating immune complexes. The inflammatory nature of these reactions, involving multiple organ systems simultaneously, contrasts sharply with predictable pharmacological side effects that typically affect specific target organs. Treatment involves drug discontinuation, anti-inflammatory medications, and sometimes corticosteroids for severe cases, with most patients recovering completely once the offending drug is eliminated.
4. Type IV Delayed-Type Hypersensitivity - T-Cell Mediated Responses
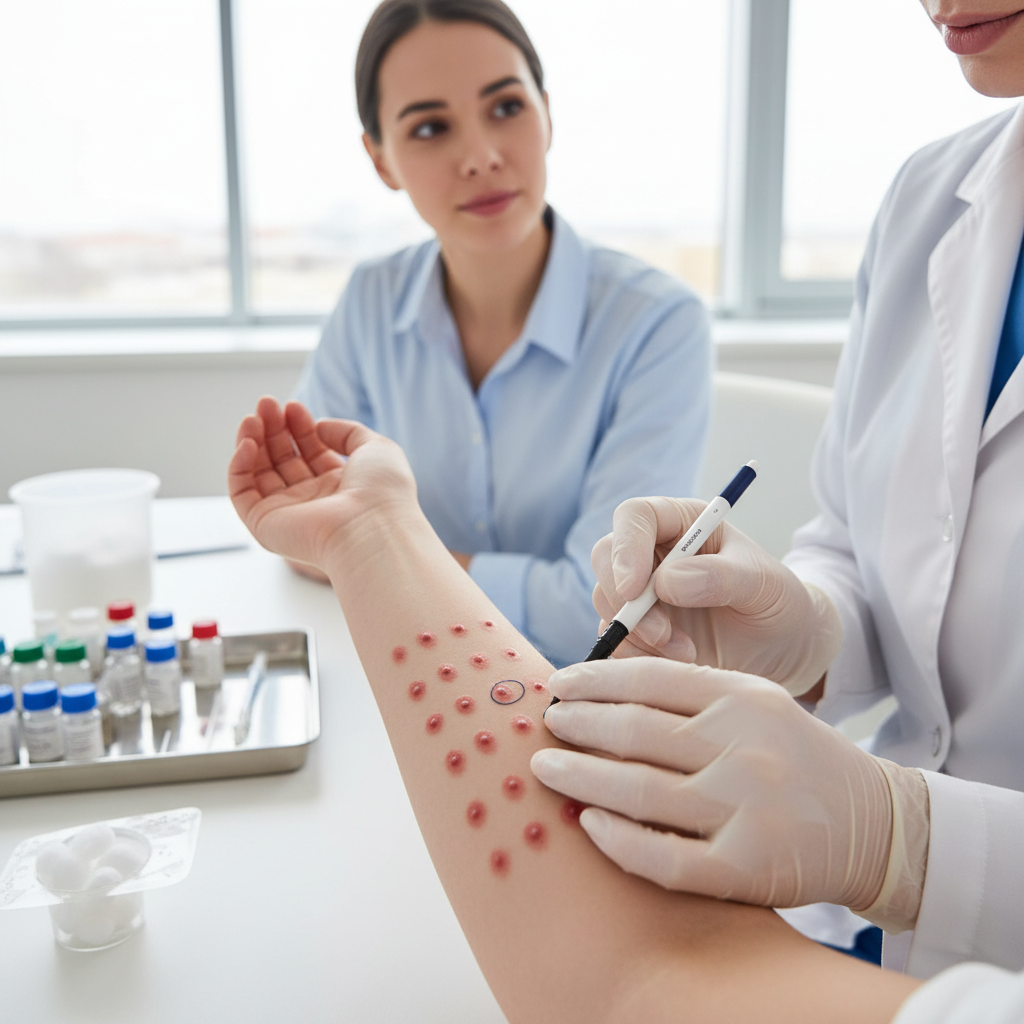
Type IV hypersensitivity reactions, also known as delayed-type hypersensitivity or T-cell mediated reactions, represent a distinct category of drug allergies that develop 48-72 hours or even weeks after drug exposure. Unlike other hypersensitivity types that involve antibodies, Type IV reactions are mediated by sensitized T-lymphocytes that recognize drug-modified proteins as foreign antigens. Upon re-exposure, these T-cells proliferate and release inflammatory cytokines, recruiting macrophages and other inflammatory cells to the site of reaction. The most common manifestation is allergic contact dermatitis, but more severe forms include Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), and drug reaction with eosinophilia and systemic symptoms (DRESS). Drugs frequently implicated include anticonvulsants (phenytoin, carbamazepine), allopurinol, sulfonamides, and certain antibiotics. The delayed onset and T-cell mediated pathophysiology clearly differentiate these reactions from immediate side effects, which occur through direct pharmacological mechanisms. Diagnosis often relies on patch testing, lymphocyte transformation tests, and clinical presentation patterns. The cellular immune response involved in Type IV reactions can cause extensive tissue damage, particularly in severe cutaneous adverse reactions, making early recognition and drug discontinuation crucial for preventing potentially fatal outcomes.
5. Severe Cutaneous Adverse Reactions (SCARs) - Life-Threatening Skin Manifestations
Severe cutaneous adverse reactions represent a spectrum of life-threatening drug-induced skin conditions that include Stevens-Johnson syndrome, toxic epidermal necrolysis, and drug reaction with eosinophilia and systemic symptoms (DRESS). These reactions are characterized by extensive skin necrosis, mucosal involvement, and systemic complications that can result in mortality rates ranging from 10-50% depending on the specific condition and extent of involvement. SJS and TEN involve widespread keratinocyte apoptosis leading to epidermal detachment, while DRESS presents with a more gradual onset featuring fever, skin eruption, lymphadenopathy, and internal organ involvement including hepatitis, nephritis, and pneumonitis. The pathophysiology involves complex immune mechanisms including cytotoxic T-lymphocyte activation, natural killer cell involvement, and release of cytolytic proteins such as granulysin and perforin. High-risk medications include anticonvulsants, allopurinol, sulfonamides, and certain antibiotics, with genetic factors such as HLA allotypes playing a significant role in susceptibility. These severe reactions differ fundamentally from common drug side effects in their immune-mediated pathogenesis, potential for systemic organ involvement, and high mortality risk. Early recognition is crucial, as prompt discontinuation of the causative drug and supportive care in specialized burn units can significantly improve outcomes. The distinction from routine side effects is critical, as these reactions require immediate emergency management and long-term avoidance of the offending drug class.
6. Cross-Reactivity Patterns and Structural Similarities in Drug Allergies

Cross-reactivity in drug allergies occurs when patients allergic to one medication also react to structurally similar drugs, representing a critical clinical consideration that distinguishes allergic reactions from typical side effects. This phenomenon is based on shared chemical structures or similar three-dimensional configurations that allow the immune system to recognize different drugs as the same antigenic threat. The most well-documented example is penicillin cross-reactivity, where patients allergic to penicillin may also react to cephalosporins, carbapenems, and monobactams due to shared beta-lactam ring structures, though the actual cross-reactivity rates are lower than historically believed. Sulfonamide cross-reactivity presents another complex pattern, where reactions to sulfonamide antibiotics may or may not predict reactions to non-antibiotic sulfonamides like furosemide or sulfonylureas, depending on the specific chemical moiety involved in the allergic response. Understanding cross-reactivity patterns is essential for safe prescribing practices and differs significantly from side effect profiles, which are typically drug-specific and related to individual pharmacological properties. Genetic factors, particularly HLA allotypes, can influence cross-reactivity patterns, as seen with abacavir hypersensitivity and HLA-B*5701. Clinical assessment of cross-reactivity requires detailed allergy histories, consideration of chemical structures, and sometimes specialized testing to determine safe alternative medications, emphasizing the immune-mediated nature of these reactions versus predictable pharmacological effects.
7. Diagnostic Approaches - Distinguishing Allergies from Side Effects

Accurate diagnosis of drug allergies requires a systematic approach that combines detailed clinical history, physical examination, laboratory testing, and sometimes specialized procedures to differentiate true immune-mediated reactions from side effects or other adverse drug reactions. The clinical history remains the cornerstone of diagnosis, focusing on the temporal relationship between drug administration and symptom onset, the nature and severity of symptoms, previous exposures, and family history of drug allergies. Physical examination during acute reactions can reveal characteristic findings such as urticaria, angioedema, or signs of anaphylaxis that are distinctly different from typical side effects. Laboratory investigations may include complete blood counts to detect cytopenias in Type II reactions, complement levels and immune complex assays for Type III reactions, and tryptase levels during suspected anaphylaxis. Specialized testing includes skin prick tests and intradermal tests for immediate hypersensitivity reactions, patch testing for delayed reactions, and drug provocation tests under controlled conditions when the diagnosis remains uncertain. In vitro tests such as basophil activation tests and lymphocyte transformation tests are emerging as valuable diagnostic tools. The diagnostic approach for drug allergies is fundamentally different from evaluating side effects, which typically rely on dose-response relationships, pharmacokinetic factors, and known pharmacological mechanisms. Proper diagnosis is crucial for patient safety, as misdiagnosis can lead to unnecessary drug avoidance or, conversely, dangerous re-exposure to truly allergenic medications.
8. Management Strategies and Emergency Interventions

Management of drug allergies requires immediate recognition, prompt intervention, and long-term preventive strategies that differ significantly from the approach to managing drug side effects. Acute management depends on the type and severity of the allergic reaction, with anaphylaxis requiring immediate epinephrine administration, airway management, intravenous fluids, and intensive monitoring in an emergency setting. For less severe reactions like urticaria or localized swelling, treatment may involve antihistamines, topical or systemic corticosteroids, and symptomatic support while ensuring complete discontinuation of the offending medication. Severe cutaneous adverse reactions require specialized care in burn units or intensive care settings, with emphasis on fluid and electrolyte management, infection prevention, and wound care. The management approach for drug allergies contrasts sharply with side effect management, which often involves dose reduction, timing modifications, or supportive care while continuing the medication if benefits outweigh risks. Long-term management includes patient education about allergy identification, medical alert jewelry or documentation, and development of comprehensive allergy lists that include cross-reactive medications. Desensitization protocols may be considered for patients who require treatment with medications to which they are allergic, particularly in cases where no suitable alternatives exist. Emergency action plans should be developed for patients with histories of severe reactions, including prescription of epinephrine auto-injectors and clear instructions for emergency situations, emphasizing the potentially life-threatening nature of true drug allergies versus manageable side effects.
9. Prevention and Future Directions in Drug Allergy Management

Prevention of drug allergies represents a multifaceted approach involving patient education, healthcare provider awareness, genetic screening, and emerging technologies that distinguish this field from routine side effect prevention. Primary prevention focuses on avoiding unnecessary drug exposure, using the narrowest spectrum agents when possible, and implementing careful prescribing practices that consider individual risk factors and previous allergic reactions. Genetic testing is becoming increasingly important, particularly for drugs with strong HLA associations such as abacavir (HLA-B*5701), carbamazepine (HLA-B*1502 in Asian populations), and allopurinol (HLA-B*5801), allowing for personalized medicine approaches that can prevent severe reactions before they occur. Electronic health records and clinical decision support systems are being developed to alert healthcare providers to potential allergic reactions and cross-reactivities, improving patient safety through technology integration. Patient education remains crucial, emphasizing the importance of accurate allergy reporting, understanding the difference between allergies and side effects, and proper use of emergency medications when prescribed. Future directions include development of better diagnostic tests, improved understanding of drug allergy mechanisms, and novel therapeutic approaches such as modified drug formulations that reduce allergenic potential. Research into biomarkers for predicting drug allergies and personalized desensitization protocols holds promise for improving patient care. The prevention of drug allergies requires a comprehensive, individualized approach that considers immune-mediated mechanisms, genetic factors, and patient-specific risk factors, fundamentally different from preventing dose-dependent side effects through standard pharmacological monitoring and dose adjustments.