10 Airborne Diseases and the Conditions That Accelerate Their Spread
7. Chickenpox and Shingles - The Dual-Phase Viral Challenge
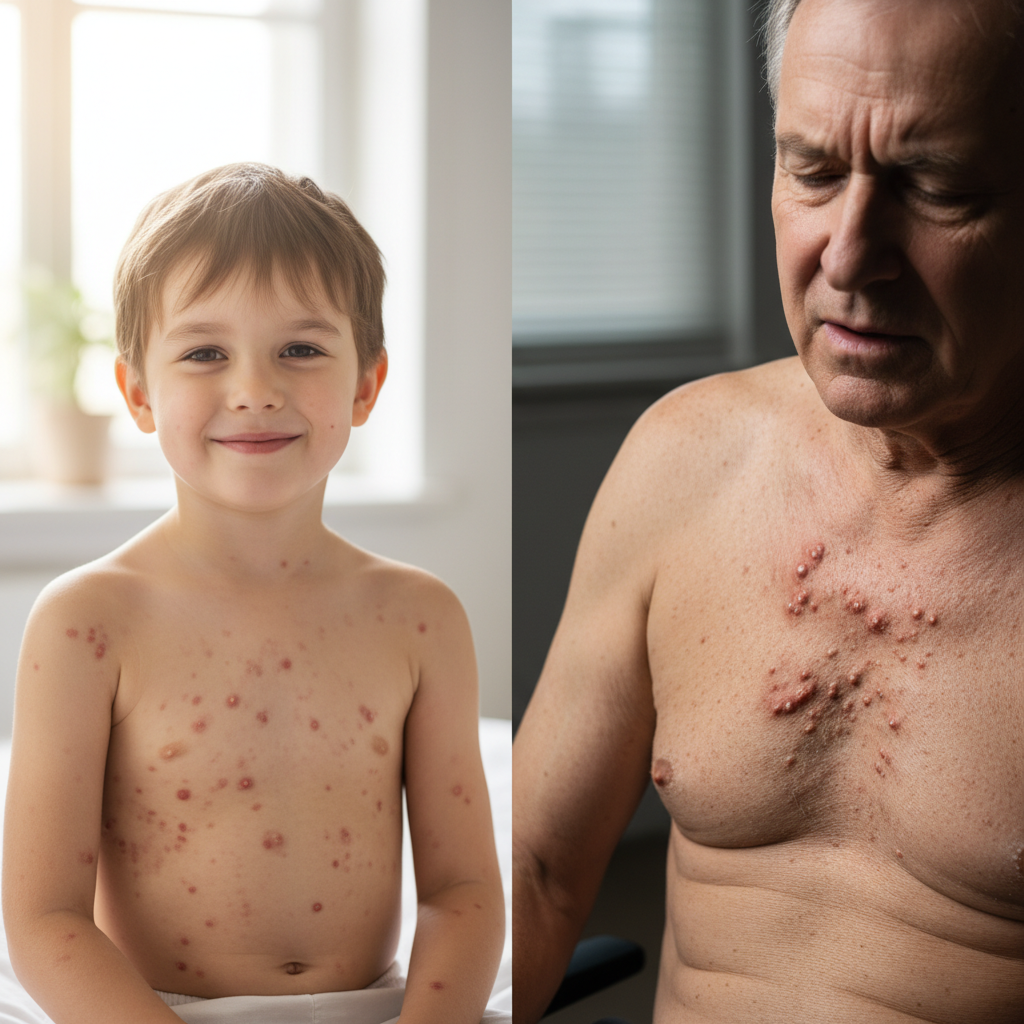
Varicella-zoster virus (VZV) presents a unique airborne transmission challenge through its dual manifestation as chickenpox (primary infection) and shingles (reactivation), creating ongoing transmission risks throughout an individual's lifetime. Chickenpox spreads extremely efficiently through respiratory droplets and aerosols, with the virus remaining viable in air for extended periods and capable of traveling significant distances through ventilation systems. The disease's high contagiosity, with attack rates approaching 90% in susceptible household contacts, makes outbreak control particularly challenging in schools and childcare facilities. Seasonal patterns typically show increased transmission during late winter and early spring in temperate climates, correlating with indoor crowding and environmental conditions favoring viral survival. Age-related susceptibility patterns show that while chickenpox primarily affects children, adult infections tend to be more severe, creating healthcare management challenges. Immunocompromised individuals face particular risks from both primary infection and reactivation, with disseminated disease potentially proving fatal without appropriate treatment. Healthcare settings require strict airborne precautions for both chickenpox and disseminated shingles cases, as nosocomial transmission can affect vulnerable patients and susceptible staff members. The virus's ability to remain dormant in nerve ganglia and reactivate as shingles creates ongoing transmission potential, particularly among elderly populations where reactivation rates increase significantly. Vaccination programs have dramatically reduced chickenpox incidence, but breakthrough infections can still occur and may present with atypical symptoms, complicating diagnosis and control efforts. International travel can facilitate virus spread between populations with different vaccination policies and natural immunity levels.
8. Aspergillosis - The Fungal Airborne Menace
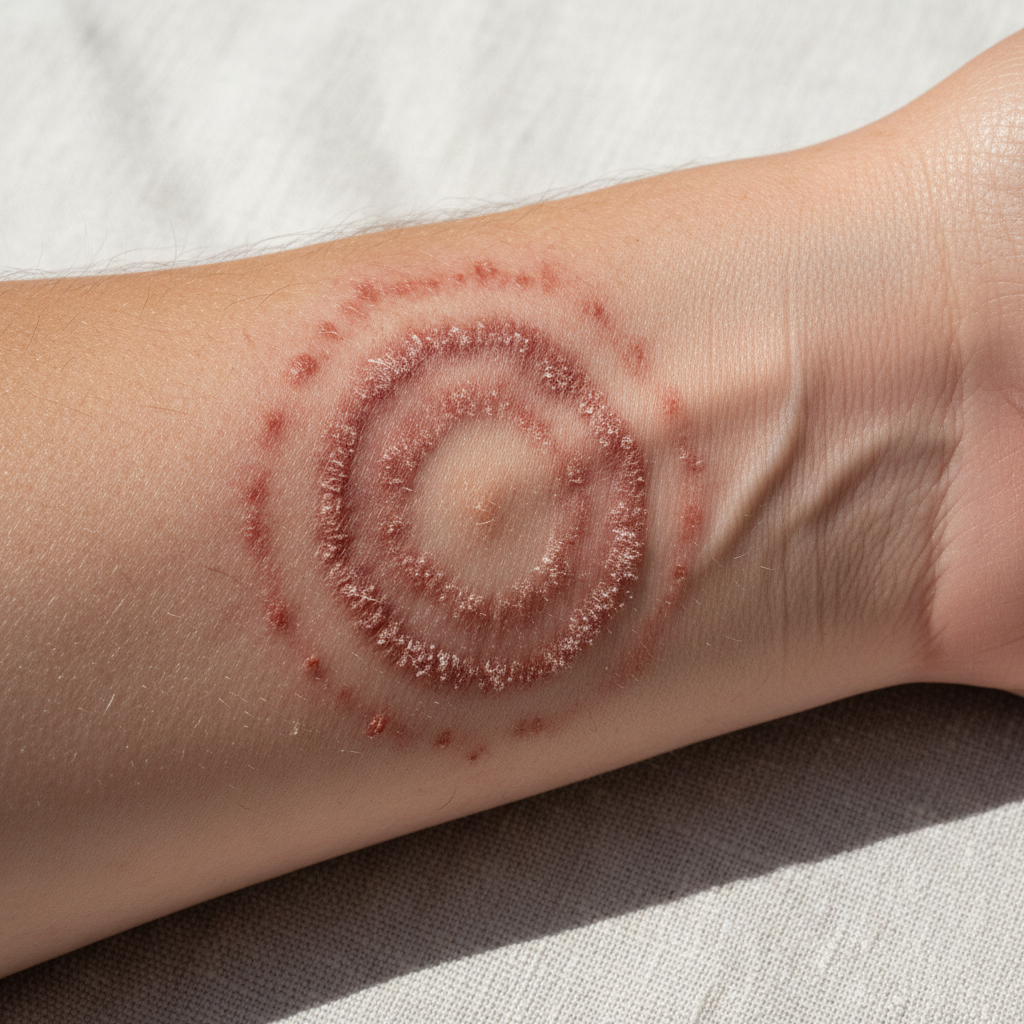
Aspergillosis represents a significant category of airborne fungal diseases caused by Aspergillus species, with transmission occurring through inhalation of ubiquitous environmental spores that become problematic under specific host and environmental conditions. Unlike bacterial or viral airborne diseases, Aspergillus spores are constantly present in outdoor and indoor environments, making exposure inevitable but infection dependent on individual susceptibility factors and spore concentration levels. Construction activities, renovation projects, and soil disturbance dramatically increase airborne spore concentrations, creating high-risk exposure scenarios particularly dangerous for immunocompromised individuals. Healthcare facilities face unique challenges in preventing aspergillosis, requiring specialized air filtration systems, positive pressure rooms, and strict environmental controls during construction or maintenance activities. Seasonal variations in outdoor spore counts, typically peaking during dry, windy conditions in late summer and fall, influence infection patterns and guide preventive measures for at-risk populations. Indoor environments can harbor Aspergillus growth in damp areas, ventilation systems, and organic materials, creating ongoing exposure risks that require environmental assessment and remediation. Immunocompromised patients, including those undergoing chemotherapy, organ transplant recipients, and individuals with chronic granulomatous disease, face life-threatening invasive infections with mortality rates exceeding 50% in some populations. Agricultural workers and individuals involved in composting or handling organic materials experience occupational exposure risks, particularly when protective equipment is inadequate. Climate change and urbanization patterns may alter environmental Aspergillus distribution and concentration, potentially affecting future infection patterns and geographic risk areas. The fungus's resistance to many antifungal agents and ability to form biofilms complicate treatment efforts and environmental control measures.