12 Zoonotic Diseases Transmitted Between Animals and Humans
7. West Nile Virus - The Mosquito-Borne Invader
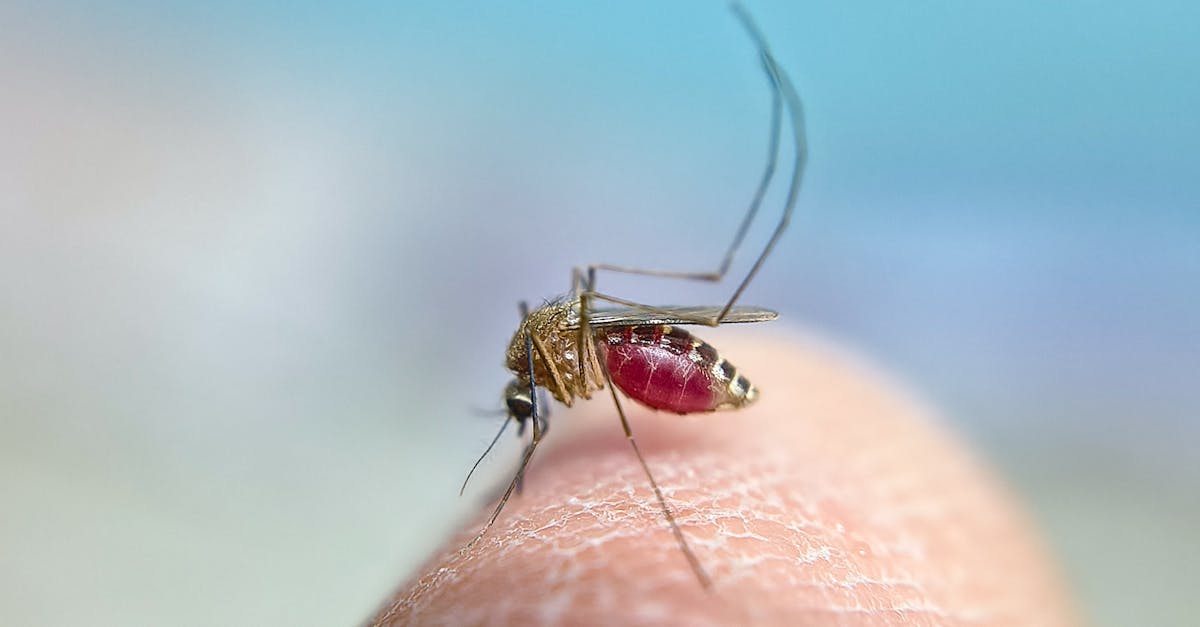
West Nile virus represents a paradigmatic example of how globalization and climate change can facilitate the rapid geographic expansion of vector-borne zoonotic diseases, transforming from a relatively obscure pathogen endemic to Africa, Asia, and Europe into a major public health concern across North America within just a few years of its introduction. This flavivirus maintains a complex enzootic transmission cycle involving mosquitoes, primarily Culex species, as vectors and birds as amplifying hosts, with humans and other mammals serving as incidental dead-end hosts that typically do not develop sufficient viremia to infect feeding mosquitoes. The virus's introduction to North America, first detected in New York City in 1999, likely occurred through infected mosquitoes or birds transported via international travel or trade, and its subsequent rapid spread across the continent demonstrated the virus's remarkable adaptability to new environments and vector species. Wild birds, particularly corvids such as crows and jays, serve as highly susceptible amplifying hosts and often experience high mortality rates, making dead bird surveillance an important component of West Nile virus monitoring programs. The clinical spectrum of West Nile virus infection in humans ranges from asymptomatic infection in approximately 80% of cases to mild febrile illness (West Nile fever) in about 20% of cases, with less than 1% of infected individuals developing severe neuroinvasive disease such as encephalitis, meningitis, or acute flaccid paralysis. Advanced age represents the most significant risk factor for severe disease, with individuals over 60 years old having substantially higher rates of hospitalization and death, while immunocompromised individuals also face increased risks of severe complications. The absence of specific antiviral treatments or vaccines for human use makes prevention the primary strategy for controlling West Nile virus, focusing on mosquito control measures, elimination of breeding sites, personal protective measures to avoid mosquito bites, and surveillance systems that monitor virus activity in mosquito and bird populations to provide early warning of increased transmission risk.
8. Plague - The Historic Pandemic Agent

Plague, caused by the gram-negative bacterium Yersinia pestis, stands as one of history's most devastating zoonotic diseases, responsible for three major pandemics that fundamentally altered the course of human civilization, including the Justinian Plague of the 6th century, the Black Death of the 14th century that killed an estimated one-third of Europe's population, and the modern pandemic that began in the 19th century and continues today in endemic foci worldwide. The bacterium maintains complex enzootic cycles involving wild rodents as reservoir hosts and fleas as vectors, with over 200 mammalian species capable of serving as hosts, though ground squirrels, prairie dogs, marmots, and other rodents represent the primary maintenance hosts in different geographic regions. The transmission to humans typically occurs through the bite of infected fleas, particularly the oriental rat flea (Xenopsylla cheopis), though direct contact with infected animals, inhalation of respiratory droplets from patients with pneumonic plague, or consumption of contaminated meat can also result in infection. The clinical manifestations of plague vary depending on the route of infection and include bubonic plague characterized by painful lymphadenopathy (buboes), septicemic plague with systemic infection and potential disseminated intravascular coagulation, and pneumonic plague involving the lungs, which represents the most dangerous form due to its potential for person-to-person transmission and rapid progression to death if untreated. Modern plague cases occur primarily in rural areas of the western United States, Madagascar, the Democratic Republic of Congo, and Peru, with most human infections resulting from exposure to infected wild rodents or their fleas during outdoor activities such as hunting, camping, or occupational exposure. The bacterium's potential as a bioterrorism agent has raised additional concerns due to its high virulence, potential for aerosol dissemination, and the possibility of developing antibiotic-resistant strains, though naturally occurring plague remains susceptible to several antibiotics including streptomycin, gentamicin, doxycycline, and ciprofloxacin when treatment is initiated promptly.