8 Drug Allergy Types and How Reactions Differ from Side Effects
3. Type III Immune Complex Reactions - The Inflammatory Cascade
Type III hypersensitivity reactions involve the formation of immune complexes between drugs or their metabolites and circulating antibodies, typically IgG, which then deposit in tissues and activate complement, leading to inflammatory damage. These reactions usually develop 1-3 weeks after drug initiation and are characterized by serum sickness-like syndrome, featuring fever, arthralgia, lymphadenopathy, and skin rashes. The pathophysiology involves the formation of small immune complexes that circulate and deposit in blood vessel walls, joints, kidneys, and skin, where they activate complement and attract neutrophils, leading to tissue inflammation and damage. Drugs commonly associated with Type III reactions include sulfonamides, penicillins, and certain biologics. The clinical presentation often includes vasculitis, glomerulonephritis, and arthritis, which can be distinguished from drug side effects by the presence of immune complex deposition and complement consumption. Laboratory findings typically show decreased complement levels (C3, C4), elevated erythrocyte sedimentation rate, and sometimes circulating immune complexes. The inflammatory nature of these reactions, involving multiple organ systems simultaneously, contrasts sharply with predictable pharmacological side effects that typically affect specific target organs. Treatment involves drug discontinuation, anti-inflammatory medications, and sometimes corticosteroids for severe cases, with most patients recovering completely once the offending drug is eliminated.
4. Type IV Delayed-Type Hypersensitivity - T-Cell Mediated Responses
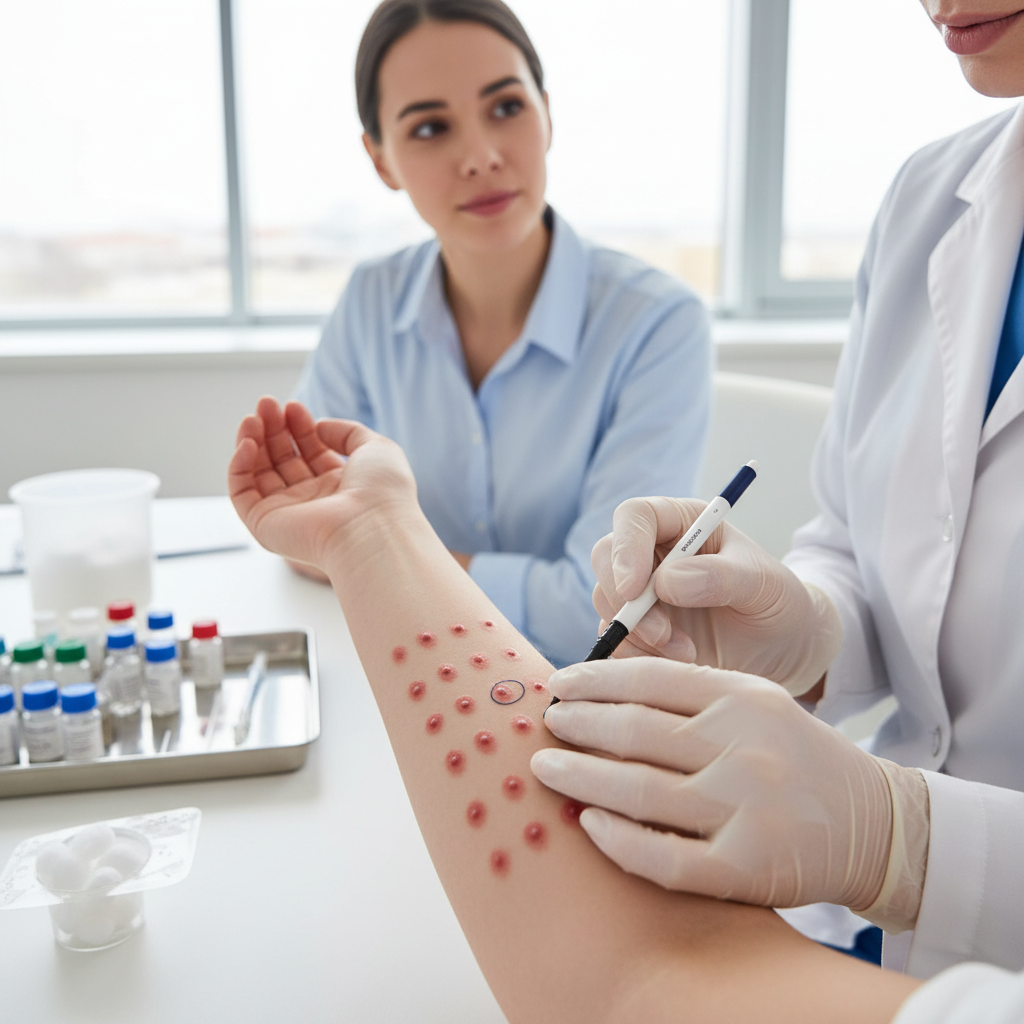
Type IV hypersensitivity reactions, also known as delayed-type hypersensitivity or T-cell mediated reactions, represent a distinct category of drug allergies that develop 48-72 hours or even weeks after drug exposure. Unlike other hypersensitivity types that involve antibodies, Type IV reactions are mediated by sensitized T-lymphocytes that recognize drug-modified proteins as foreign antigens. Upon re-exposure, these T-cells proliferate and release inflammatory cytokines, recruiting macrophages and other inflammatory cells to the site of reaction. The most common manifestation is allergic contact dermatitis, but more severe forms include Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), and drug reaction with eosinophilia and systemic symptoms (DRESS). Drugs frequently implicated include anticonvulsants (phenytoin, carbamazepine), allopurinol, sulfonamides, and certain antibiotics. The delayed onset and T-cell mediated pathophysiology clearly differentiate these reactions from immediate side effects, which occur through direct pharmacological mechanisms. Diagnosis often relies on patch testing, lymphocyte transformation tests, and clinical presentation patterns. The cellular immune response involved in Type IV reactions can cause extensive tissue damage, particularly in severe cutaneous adverse reactions, making early recognition and drug discontinuation crucial for preventing potentially fatal outcomes.